Table of Contents
- Why Toxic Ingestion Emergencies Demand Immediate Knowledge
- Recognizing Signs of Poisoning in Children
- The Critical First 60 Seconds: What You Must Do
- Calling Poison Control: Getting Expert Guidance Fast
- Managing the Child Until Emergency Responders Arrive
- When to Perform CPR or Rescue Breathing
- Post-Emergency Care and Medical Follow-Up
- Building Your Emergency Response Team at Work or Home
- Certification Training That Prepares You for Real Emergencies
- Why Healthcare Providers Choose Our Specialized Programs
- Frequently Asked Questions (FAQ)
Why Toxic Ingestion Emergencies Demand Immediate Knowledge
Every year, poison control centers across the country receive over 2 million calls involving toxic ingestions, with children under six accounting for a significant portion. When a child swallows a toxic substance, the first few minutes determine whether outcomes are minor or catastrophic. You may have only seconds to act before absorption occurs, and knowing the right steps transforms panic into purposeful action.
Healthcare professionals, childcare providers, and parents who understand poisoning response protocols save lives. Whether you work in emergency medicine, pediatrics, nursing, or oversee young children in any setting, this knowledge bridges the gap between the moment of ingestion and professional medical intervention. We’ve seen countless situations where trained individuals made the critical difference simply because they knew what to do and what to avoid.
Toxic substances range from household cleaners and medications to pesticides, alcohol, and plants. Children’s curiosity combined with their smaller body size means even small quantities can cause serious harm. The stakes are high, but your preparedness directly controls the outcome.
Recognizing Signs of Poisoning in Children
Signs of poisoning emerge quickly but vary widely depending on the substance and amount ingested. Early recognition allows you to act before symptoms progress to life-threatening levels. Watch for these common indicators:
Behavioral and neurological signs include drowsiness, agitation, confusion, loss of consciousness, or seizures. Your child may become unusually calm or hyperactive, slur speech, or lose coordination. Gastrointestinal symptoms include nausea, vomiting, abdominal pain, diarrhea, or visible blood in vomit or stool. Respiratory changes like rapid breathing, shallow breathing, or difficulty breathing demand immediate attention.
Physical symptoms vary by toxin: pinpoint or dilated pupils, skin rashes or burns around the mouth, chemical odor on breath, excessive drooling, or unusual skin color (pale, blue, or flushed). Some children show no immediate signs despite serious ingestion, which is why professional evaluation matters even when symptoms seem absent.
Don’t wait for obvious signs. If you suspect ingestion of any substance that shouldn’t be consumed, treat it as an emergency. In Fremont, Sacramento, and across our service areas in California, we train professionals to recognize these patterns and act decisively rather than hesitate while watching for confirmation.
The Critical First 60 Seconds: What You Must Do
Your first minute sets the trajectory for the entire emergency response. Immediately move the child away from the poison source and ensure their airway is clear. If the child is responsive and can swallow, keep them calm while you gather information about what was ingested, when, and approximately how much.
Never induce vomiting. This outdated approach can cause additional harm by bringing caustic substances back through the esophagus or causing aspiration into the lungs. Similarly, do not try to neutralize the poison with water or milk unless poison control specifically instructs you to do so. Each substance requires different handling.
Do this in your first 60 seconds:
- Remove any remaining toxic substance from the child’s mouth and hands
- Note the product name, ingredient list, and any visible container information
- Document the time of ingestion as accurately as possible
- Keep the original container nearby for reference
- Contact poison control immediately (do not wait to see if symptoms develop)
- Stay with the child and keep them warm and calm
If the child is unconscious or seizing, place them on their side in the recovery position to prevent aspiration. Check that they’re breathing and have a pulse. Your knowledge of basic life support becomes critical if poisoning affects respiration or heart function. Facilities in Oaklanland, San Jose, and locations across Northern and Central California train staff on these exact scenarios during our specialized courses.
Calling Poison Control: Getting Expert Guidance Fast
Poison Control in the United States operates 24/7 at 1-800-222-1222. Call immediately when you suspect ingestion. This is not a resource of last resort; it’s your first call alongside or even before 911 in many cases. Poison control specialists have immediate access to toxin databases and provide real-time guidance tailored to the specific substance and child.
When you call, have this information ready:

- Child’s age and weight
- Exact name of the substance (read the label)
- Time of ingestion
- Amount ingested (or best estimate)
- Any symptoms currently present
- Current location and access to emergency services
Poison control will advise whether you need emergency transport, can manage at home with monitoring, or should visit an urgent care facility. They may recommend observation periods, activated charcoal, or specific supportive care. Follow their guidance precisely. If they recommend emergency transport, call 911 immediately.
Your poison control conversation is documented and shared with emergency responders if the child is transported, ensuring continuity of care. Never feel embarrassed calling; they handle thousands of inquiries monthly and take every call seriously. The specialists understand that exposure to toxic substances is often accidental and their role is to help, not judge.
Managing the Child Until Emergency Responders Arrive
Once you’ve called poison control and emergency services, your role shifts to stabilization and comfort. Keep the child calm and still, as movement increases heart rate and can accelerate absorption of some toxins. Speak in reassuring tones and avoid alarming language; children sense panic and respond with increased distress.
Monitor breathing and consciousness continuously. Count respirations (normal is 20-30 per minute for young children) and check skin color and temperature. Document any changes or new symptoms and report them to emergency responders when they arrive. If the child becomes unconscious, immediately perform a head-tilt, chin-lift maneuver to open the airway and assess breathing.
Position matters significantly. A conscious child should sit upright or recline slightly to prevent vomiting and aspiration. An unconscious, breathing child belongs in the recovery position (on their side with head tilted back slightly). Never leave the child unattended. Keep the toxic substance container visible for paramedics.
Have your phone nearby and be ready to provide rapid updates to 911 dispatch. If the ingestion involved a corrosive substance (drain cleaner, oven cleaner), do not attempt to rinse the mouth or induce vomiting; simply keep the child calm and waiting for professionals. Healthcare professionals in Bakersfield, Fresno, and throughout our California network understand these protocols because they practice them in our emergency response training programs.
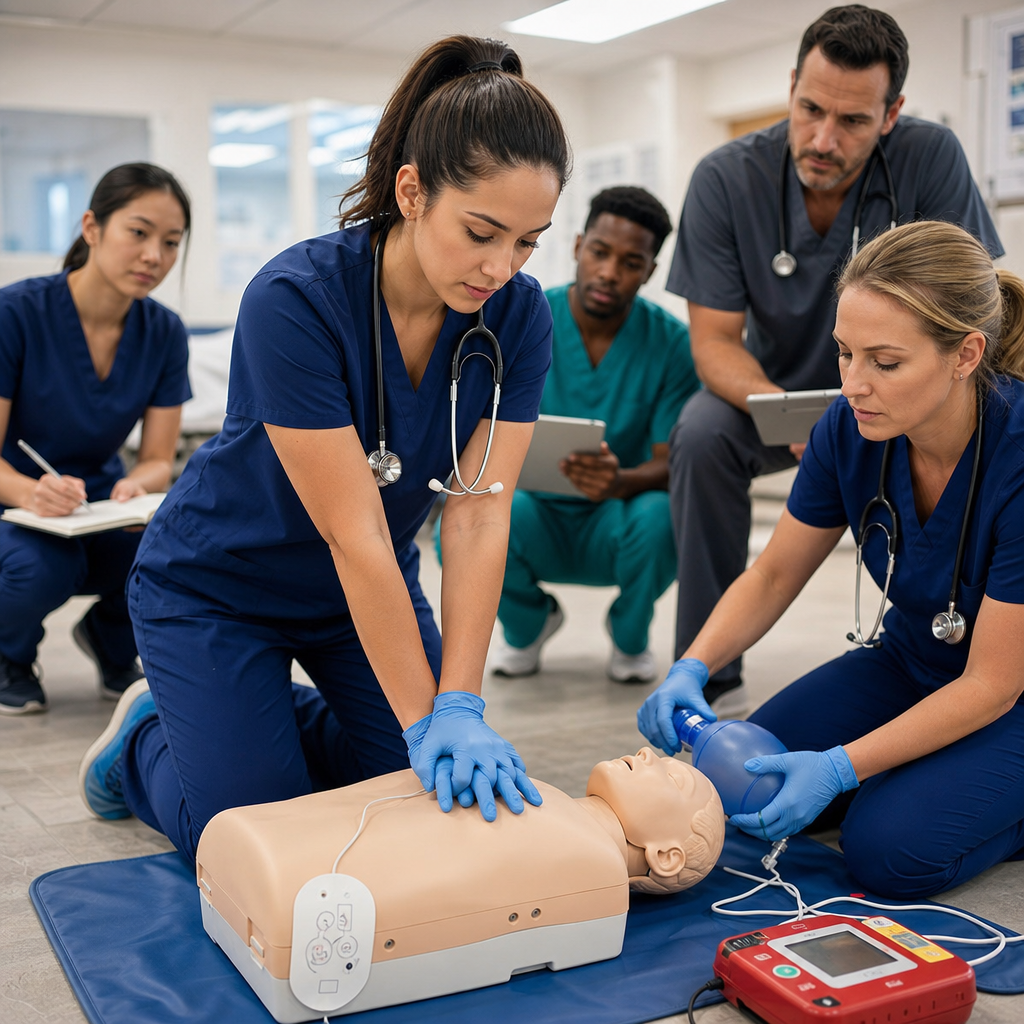
When to Perform CPR or Rescue Breathing
If the child becomes unresponsive and stops breathing, or shows no signs of circulation, CPR becomes necessary. Check for responsiveness by tapping gently and calling the child’s name. Open the airway and look for breathing for no more than 10 seconds. If breathing is absent or gasping only, begin CPR immediately.
For infants (under 1 year), use two fingers to provide chest compressions at the center of the chest, compressing about one-third of chest depth at a rate of 100-120 compressions per minute. For children 1-8 years old, use one or two hands to maintain the same rate and depth. Alternate 30 compressions with 2 rescue breaths, allowing the chest to fully re-expand between compressions.
Continue CPR until emergency responders take over or the child shows clear signs of life. Do not pause to check for a pulse unless you’re trained and confident; if you’re unsure, keep performing CPR. Poison-related cardiac arrest may be reversible with prompt, continuous CPR.
If you’re untrained or unsure about rescue breathing, hands-only CPR (compressions without breathing) is extremely effective and preferred by many organizations. Push hard and fast on the center of the chest. Emergency dispatch can provide real-time coaching if you call 911.
Certification in pediatric BLS or PALS prepares you for these exact scenarios with hands-on manikin practice. Our instructors across locations including Walnut Creek, Danville, and Livermore emphasize that real-world performance under stress depends on repeated practice before an actual emergency occurs.
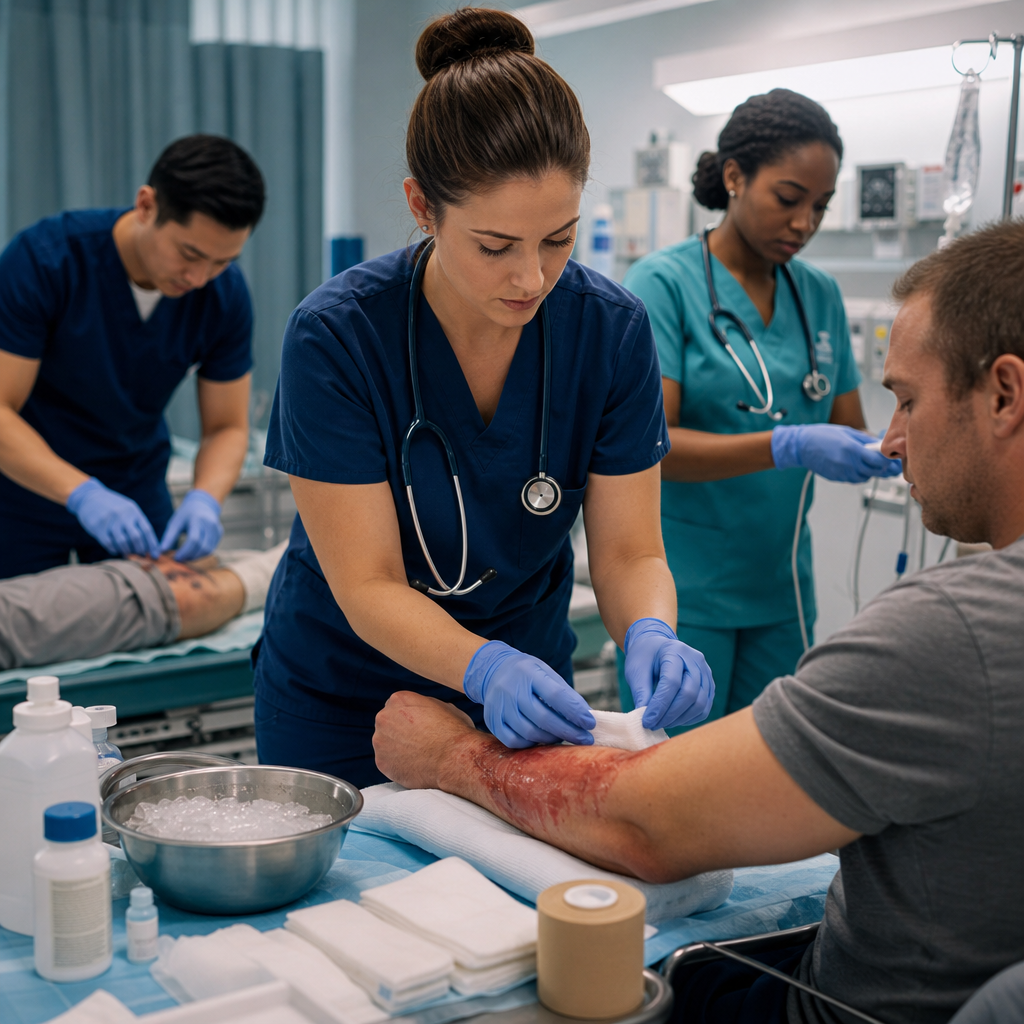
Post-Emergency Care and Medical Follow-Up
Once emergency responders take over, the child will be transported to an emergency department for evaluation and ongoing treatment. Bring the container or substance name with you. Medical professionals will perform blood work, imaging, and monitoring to assess the extent of poisoning and guide treatment.
Some toxins require specific interventions like activated charcoal, gastric lavage, or specific antidotes. Others require supportive care and observation until the substance is metabolized. Stay informed and ask the medical team for updates on treatment plan, expected timeline, and follow-up appointments.
Poison control may request follow-up information about how the child responded to recommended treatment. Provide honest, detailed reports to help refine their protocols. After discharge, keep all follow-up appointments and watch for delayed symptoms, which can occur hours or days after ingestion depending on the substance.
Document the incident for your records and your family’s medical history. If you’re in a childcare setting or healthcare facility, incident reports are mandatory and serve to identify prevention gaps. Review how access to the toxic substance occurred and implement barriers to prevent recurrence.
Building Your Emergency Response Team at Work or Home

Individual knowledge is valuable, but coordinated emergency response saves more lives. If you work in healthcare, childcare, or any setting with children present, establish a clear emergency protocol that your entire team understands and practices regularly.
Identify team members trained in CPR and first aid and ensure their certifications remain current. Post poison control’s number (1-800-222-1222) prominently in every area where it might be needed. Conduct quarterly drills simulating toxic ingestion scenarios so everyone knows their role when real emergencies occur. Assign specific individuals to call 911, provide care, document information, and contact parents or guardians.
For homes with young children, store all toxic substances in locked cabinets away from reaching hands. This includes medications, cleaning products, pesticides, and even some plants. Use childproof containers and keep poison control’s number on your refrigerator and in your phone. Teach older children that unknown substances should never be tasted or touched.
Group CPR Classes at your workplace or organization ensure your entire team maintains current certifications and practices together. We offer discounted group rates across our 100+ California locations, making it affordable to certify every staff member. Organizations in San Francisco, San Jose, Sacramento, and throughout California use our programs to build cohesive response teams.
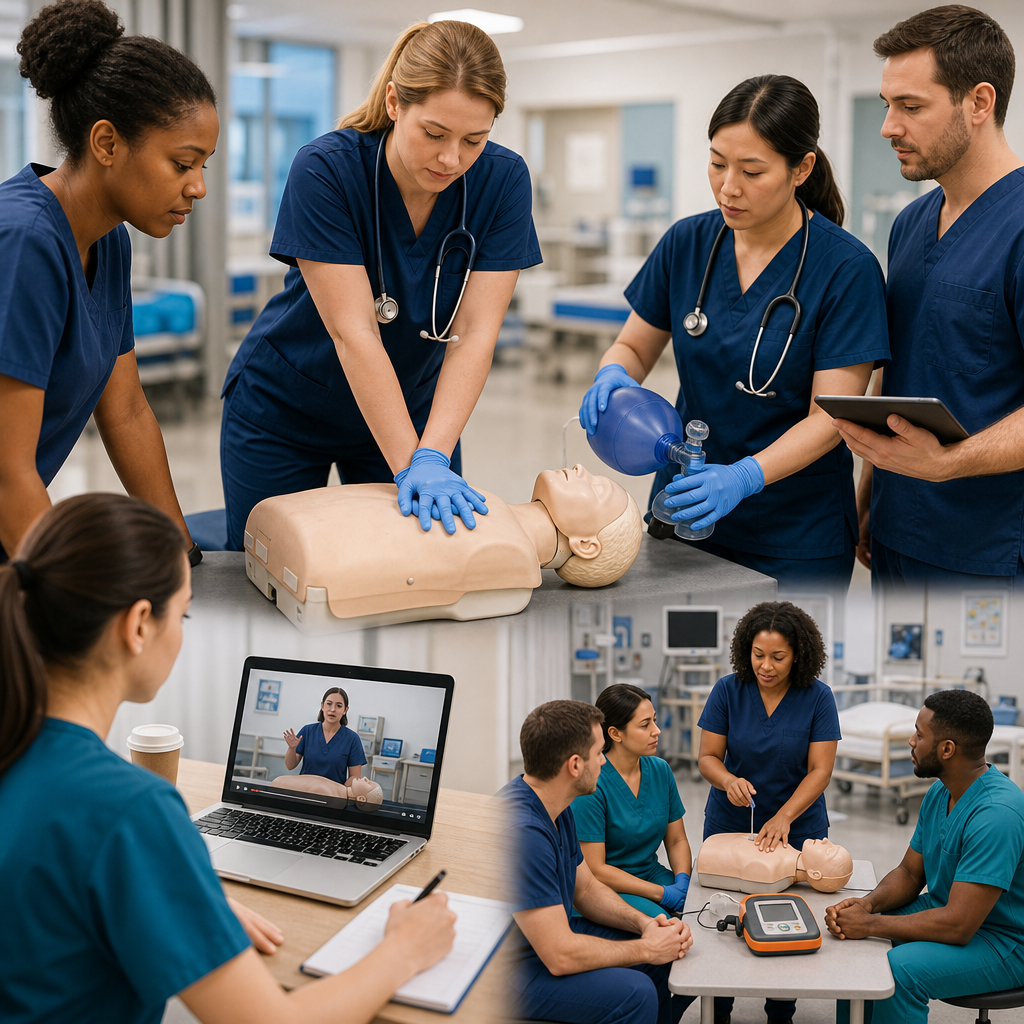
Certification Training That Prepares You for Real Emergencies
Knowing emergency procedures intellectually differs fundamentally from performing them under pressure with a real child’s life at stake. Certification training bridges that gap through scenario-based learning where you practice on realistic manikins while instructors provide immediate feedback on technique and decision-making.
We offer specialized pediatric courses including PALS (Pediatric Advanced Life Support) for healthcare providers and CPR/BLS certification for anyone working with children. Our blended learning model combines online knowledge review with in-person skills sessions where you perform actual rescue breathing, chest compressions, and emergency response protocols. This hands-on practice builds muscle memory and confidence.
Our instructors are experienced healthcare professionals who have managed real pediatric emergencies. They understand what works in controlled training settings versus in chaotic real-world situations and teach accordingly. Small class sizes allow personalized feedback on your technique. Certification is valid for two years, but we recommend annual refreshers to maintain proficiency.
Why Healthcare Providers Choose Our Specialized Programs
Healthcare professionals across California choose our training because we understand their specific needs. Nurses, dentists, EMS personnel, and pediatric specialists require certifications that meet their licensing boards’ exact requirements. Our courses are designed and taught by clinicians who practice in the specialties they teach.
We maintain low price guarantees across all our programs, with daily class availability at over 100 locations including Folsom, Concord, Pleasanton, and throughout California. Our flexible scheduling accommodates shift work, and our blended learning format lets you complete online coursework on your timeline before arriving for hands-on skills practice.
Beyond certification, we invest in your confidence. Our instructors create psychologically safe learning environments where asking questions and practicing mistakes in training builds the competence you need when real emergencies occur. We’ve trained thousands of healthcare professionals who’ve successfully managed poisoning cases, cardiac arrests, and other life-threatening emergencies because they practiced with us first.
Your next step is straightforward: visit our site to schedule your pediatric CPR or PALS certification at a location convenient to you. Whether you’re in rural areas like Visalia or Redding or urban centers like San Francisco and Oakland, we have classes available. Ensure you and your team are prepared for the emergencies no one expects but everyone hopes they’ll handle perfectly if they occur.
Register for a class today.
Frequently Asked Questions (FAQ)
How do we prepare healthcare providers to respond to pediatric poisoning emergencies?
We offer specialized training that covers toxicology recognition, immediate response protocols, and communication with poison control centers. Our courses include realistic scenario-based practice with pediatric mannequins so nurses, dentists, and EMS personnel can develop confidence before facing actual emergencies. We teach the specific techniques needed to manage airway and breathing support if a child becomes unresponsive after toxic ingestion.
What makes our certification training different for emergency response situations?
We combine blended learning with hands-on skills sessions at our 100+ California locations, allowing our students to practice critical interventions under direct instructor supervision. Our instructors draw from real emergency experience and teach you the exact sequence of actions required in the first 60 seconds of a poisoning incident. We also provide daily scheduling flexibility so you can earn your certification without disrupting your work schedule.
Can we help our entire healthcare facility stay current on pediatric emergency protocols?
Yes, we offer corporate group training with discount pricing for hospitals, clinics, dental practices, and EMS stations throughout California. We come to your location or you can attend at one of our nearby training centers, and we work with your scheduling needs to ensure your team maintains compliance with mandatory certifications.