Table of Contents
- Why Unresponsiveness During or After Exercise Demands Immediate Action
- Common Causes of Exercise-Related Collapse in Adults
- How to Recognize When Someone Needs Emergency Help
- The Critical First Steps: Assessment and Calling for Help
- Performing Effective CPR on an Unresponsive Exercise Participant
- Using Automated External Defibrillators in Emergency Situations
- Our Certified Training Programs Prepare You for Real Emergencies
- Why Healthcare Professionals Choose Our Hands-On Certification Courses
- Getting Your Emergency Response Certification Today
- Frequently Asked Questions (FAQ)
Why Unresponsiveness During or After Exercise Demands Immediate Action
An unresponsive person after exercise represents one of the most time-sensitive medical emergencies you may encounter. Whether you work in a hospital, clinic, fitness facility, or community health setting, the first few minutes following collapse or loss of consciousness directly determine survival outcomes and long-term health. Every second without proper intervention increases the risk of permanent injury or death.
Exercise-related unresponsiveness can stem from several serious conditions, many of which are reversible if treated immediately. The good news: you likely have the tools and knowledge to save a life, but only if you act decisively. We’ve trained thousands of California healthcare professionals to recognize these emergencies and respond with confidence, and that preparation makes the difference between a full recovery and tragedy.
The stakes are highest in those critical first moments before advanced life support arrives. Your rapid assessment, clear communication, and correct technique can preserve brain function and keep a patient alive until paramedics take over.
Common Causes of Exercise-Related Collapse in Adults
Several medical conditions trigger sudden unresponsiveness during or immediately after physical activity. Understanding these causes helps you anticipate what you might encounter and stay alert in high-risk environments.
Sudden cardiac arrest remains the leading cause of exercise-related collapse in adults. This occurs when the heart stops pumping effectively, cutting off blood flow to the brain within seconds. Young athletes often have undiagnosed structural heart problems like hypertrophic cardiomyopathy, while older adults may experience acute coronary events triggered by exertion.
Heat stroke represents another critical cause, particularly during outdoor activities in warm climates. California’s hot summers create real risk, especially for individuals exercising in direct sun or pushing harder than their bodies can handle. Body temperature climbs above 104 degrees Fahrenheit, damaging the central nervous system and causing loss of consciousness.
Severe dehydration and electrolyte imbalances develop during prolonged exercise without adequate fluid replacement. Symptoms progress from dizziness to confusion, and if unaddressed, lead to seizures and collapse. Exertional hyponatremia (dangerously low blood sodium) can occur even in well-intentioned athletes who overhydrate with plain water.
Vasovagal syncope causes temporary loss of consciousness when blood pressure drops suddenly in response to a trigger. Although often brief and self-resolving, syncope during exercise poses serious injury risk, especially if the person falls and strikes their head.
Hypoglycemia in individuals with diabetes or those who’ve exercised intensely without eating triggers unresponsiveness and seizures. These episodes develop rapidly and demand immediate blood glucose correction.
How to Recognize When Someone Needs Emergency Help
Your ability to quickly identify a true emergency separates appropriate response from costly delays. Watch for these clear indicators that someone requires immediate intervention.
An unresponsive person who doesn’t wake when you tap their shoulders and speak loudly needs emergency help now. Check responsiveness by shouting near their ear and gently stimulating them, but don’t assume they’re simply tired or fatigued.
Abnormal or absent breathing is the most critical sign. Normal breathing appears as regular chest rise and fall. Gasping, gurgling, irregular breathing patterns, or complete absence of chest movement all signal serious trouble. Many people mistake gasping for normal breathing, so look carefully.
Skin color changes matter too. Pale, grayish, or bluish skin indicates inadequate oxygen delivery. Check the person’s lips, face, and nail beds for these color changes, which develop quickly once breathing fails.

Unresponsiveness combined with no pulse demands immediate CPR initiation. You don’t need to be absolutely certain about a pulse to act. Modern guidelines emphasize that if someone is unresponsive and not breathing normally, begin chest compressions immediately.
Seizure activity during or after exercise represents a medical emergency. Even if the seizure appears brief, the person needs immediate evaluation because seizures during exercise can indicate heart problems, heat stroke, or neurological emergencies.
Confusion, slurred speech, or inability to follow simple commands suggest a serious event. A person who exercised, collapsed, and now seems disoriented requires emergency response even if they’re technically conscious.
The Critical First Steps: Assessment and Calling for Help
Your first 10 seconds determine whether the person receives life-saving treatment. Skip the urge to move them or search for explanations; focus on assessment and activation of emergency services.
Check responsiveness immediately. Tap both shoulders firmly and shout, “Are you okay?” Watch for any response: opening eyes, moving, or speaking. If there’s no response, proceed to the next steps without delay.
Look and listen for normal breathing while checking for a pulse simultaneously. Place two fingers on the carotid artery in the neck and watch the chest. This assessment should take no more than 10 seconds. If you’re unsure whether breathing is normal or can’t find a pulse, assume the worst and act.
Call 911 or your facility’s emergency code right now. Don’t wait for additional signs or for someone else to call. In a workplace or gym setting, immediately direct the nearest person to call for help while you begin assessment. Use speaker phone if available so you can follow the dispatcher’s instructions while maintaining access to the patient.
Request an automated external defibrillator (AED) be brought to you immediately. Have someone retrieve it while you continue assessment and prepare to begin CPR. In facilities with AEDs, knowing exactly where the nearest unit is located eliminates precious seconds of searching.
If your facility has a crash cart or emergency equipment, have someone bring it to you. Don’t leave the unresponsive person to search yourself; direct someone specific to fetch equipment and confirm they’re actually going.
Document the exact time you found the person unresponsive and when you called for help. These details matter for the paramedics and the medical record, but don’t let documentation delay your response.
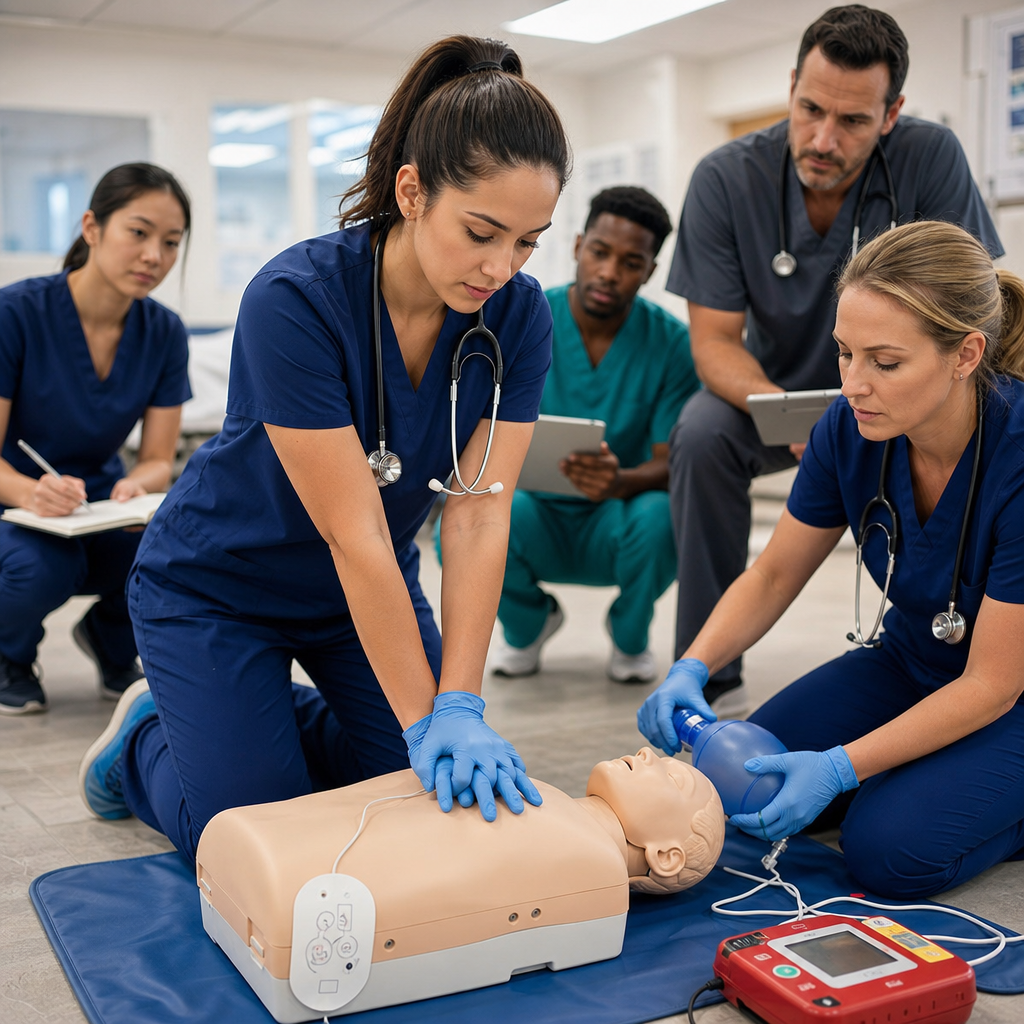
Performing Effective CPR on an Unresponsive Exercise Participant
CPR is straightforward: push hard and fast on the chest while maintaining an open airway. Modern guidelines emphasize chest compressions as the primary lifesaving intervention.
Position the person on their back on a firm surface. If they’re on a slope or soft ground, move them to flat, solid footing where you can generate adequate force. Work quickly but avoid unnecessary rough handling.
Place the heel of one hand on the center of the chest between the nipples, then place your other hand on top, interlacing fingers. Keep your arms straight and positioned directly over the person’s chest. This hand position ensures force goes straight down through the ribcage rather than at an angle.
Push hard and fast at a rate of 100 to 120 compressions per minute. This translates to roughly two compressions per second. Many find it helpful to mentally sync compressions to the beat of an upbeat song. Compress the chest at least 2 inches deep with each push, allowing the chest to fully recoil between compressions.
Maintain compressions continuously until the AED arrives and is applied, a paramedic takes over, or the person shows signs of life. If you’re alone and exhausted, keep going. Even imperfect CPR saves more lives than no CPR.
Once an AED is available, apply pads immediately while continuing chest compressions. Don’t stop compressions to prepare the pads; the person administering CPR should keep going while someone else readies the device.

If trained in rescue breathing, provide 30 compressions followed by 2 rescue breaths, then repeat. If you’re not trained in rescue breathing or uncomfortable providing it, compressions alone are equally effective and eliminate hesitation.
Switch compressors every 2 minutes if possible. Effective CPR is physically exhausting, and fresh hands maintain better compression quality. Communicate clearly: “I’ll take compressions; you watch for AED arrival.”
Using Automated External Defibrillators in Emergency Situations
An AED is one of the most powerful tools in emergency response, and using it correctly dramatically improves survival chances for cardiac arrest victims. These devices are designed for non-specialists, but proper technique matters.
Turn on the AED as soon as it arrives. You’ll see either a power button or opening the device may automatically activate it. Either way, the device will provide voice prompts guiding you through each step.
Remove the person’s chest hair if it’s dense, exposing dry skin. Some AED kits include razors for this purpose. Dry the chest area if the person is wet, as moisture prevents proper pad adhesion and creates electrical hazards.
Peel the protective backing from the adhesive pads. Apply one pad directly on the right upper chest, below the collarbone and to the right of the breastbone. Apply the second pad on the left side, along the mid-axillary line (imagine a line from the armpit down the ribcage) at the level of the lowest rib.
Push firmly on each pad to ensure complete contact with the skin. Poor pad placement reduces effectiveness, so take a second to ensure proper adhesion.
Once pads are applied, make sure no one is touching the person and announce “Analyzing” loudly. Keep everyone back from the person so the AED can complete its analysis without interference.
If the AED recommends a shock, ensure everyone is clear of the person, then press the shock button when prompted. After the shock, resume CPR immediately at a rate of 100 to 120 compressions per minute. Don’t check for responsiveness or pulse; go straight into compressions.
Follow the AED’s prompts for the next recommended shock interval, typically every 2 minutes. The device will continue to analyze and advise. Your job is to perform CPR between shocks and follow the device’s guidance until paramedics arrive.
Continue this cycle of CPR and shocks until paramedics take over or the person shows unmistakable signs of life like normal breathing and responsiveness.
Our Certified Training Programs Prepare You for Real Emergencies
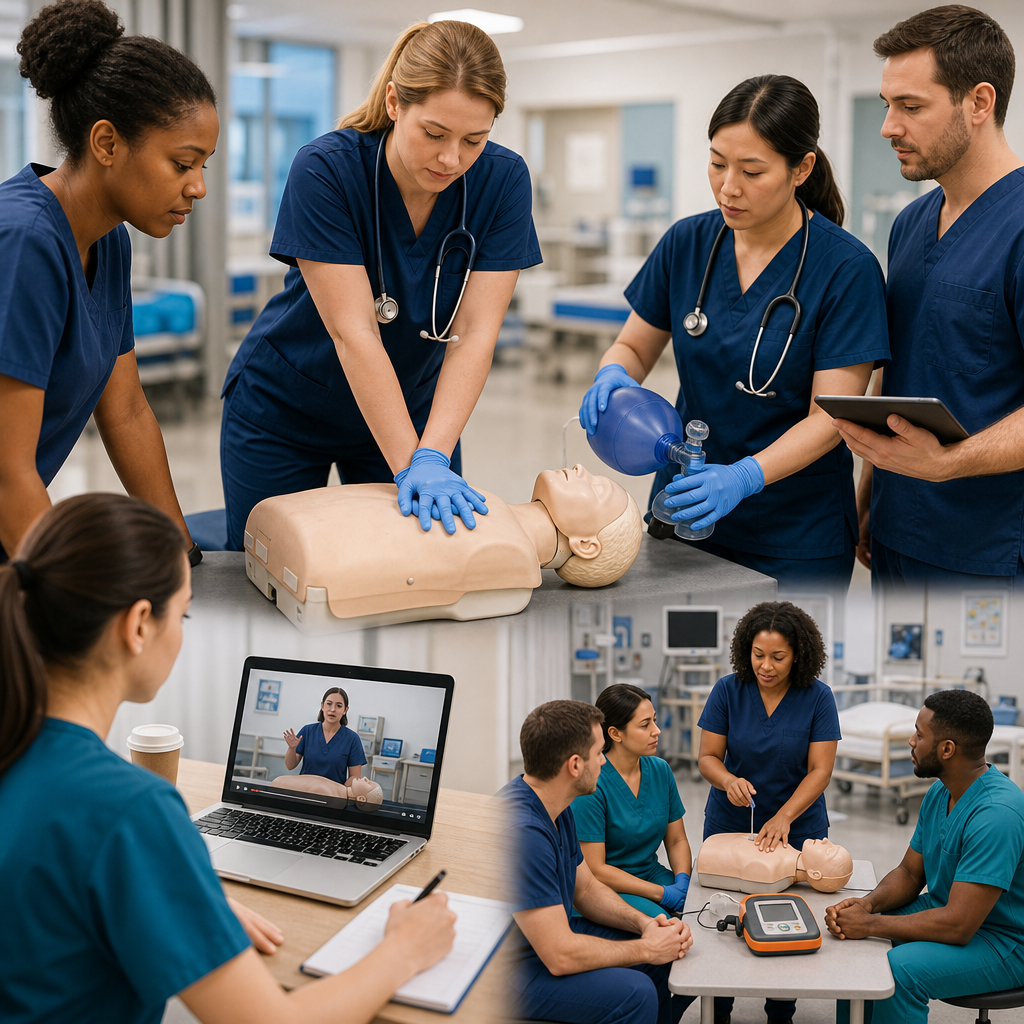
We understand that knowing CPR academically and performing it under pressure are completely different experiences. That’s why we emphasize hands-on practice with real equipment in scenarios that mimic actual emergencies. Our instructors have extensive experience in acute care settings across California, from Sacramento to San Jose, and they design every course around the situations you’ll actually face.
Our blended learning approach combines online modules covering theory with in-person skills sessions where you practice chest compressions, AED application, and rescue breathing on mannequins before ever encountering a real patient. You’ll work with the exact equipment your facility uses, whether that’s a specific AED model or ventilation devices. This familiarity eliminates hesitation when seconds count.
We offer BLS (Basic Life Support) certification for all healthcare professionals, ACLS (Advanced Cardiovascular Life Support) for nurses and emergency personnel, and specialized programs like PALS (Pediatric Advanced Life Support) for those caring for children. Each program builds practical competence through repetition and real-world scenarios, not just lecture.
All our courses are available at convenient California locations near you, with class times that work around your schedule. We offer daily BLS certification sessions and evening classes for professionals working full-time shifts. Whether you’re based in the Bay Area near Oakland or Fremont, the Central Valley near Modesto or Visalia, or Southern California locations like Bakersfield, we have training nearby.
Why Healthcare Professionals Choose Our Hands-On Certification Courses

Healthcare professionals across California trust us because we focus on practical competence, not just checking compliance boxes. Our instructors are experienced nurses, paramedics, and emergency physicians who’ve actually performed CPR in real emergencies, so they teach from real experience rather than generic scripts.
We maintain a low price guarantee, ensuring your certification costs don’t exceed what you’d pay elsewhere. Combined with our flexible scheduling and online-plus-in-person format, we make recertification accessible rather than burdensome. Many professionals complete their entire course in a single day, with online content finished the evening before.
Our CPR verification stations throughout California allow quick skill checks if you need reassurance between certifications. This gives you confidence that your technique remains sharp without committing to a full recertification course.
You’ll receive certification recognized across California’s healthcare system, whether you work for a hospital network, private practice, fitness facility, or public health agency. Our credentials satisfy licensure requirements for nurses, dentists, EMS personnel, and other regulated professionals.
Group discounts make team training affordable for clinics, gyms, and corporate wellness programs. We bring instruction directly to your location across Alameda, Contra Costa, and other California regions, reducing travel time and keeping your team together during training.
Getting Your Emergency Response Certification Today
Your next step is straightforward: visit our website at https://safetytrainingseminars.com or call to schedule a CPR and BLS certification course at a California location near you. We have classes available at over 100 locations statewide, with multiple sessions each week to accommodate your schedule.
Most professionals complete certification in a single day. Choose between in-person intensive courses or our blended approach, where you complete the online module at home and attend a 2-3 hour skills session at a convenient location like San Francisco, Berkeley, or elsewhere in Northern California.
If you need ACLS or specialized certifications beyond basic CPR, we offer those as well, with the same hands-on emphasis and convenient scheduling. Many healthcare professionals combine courses, completing BLS and ACLS certification on the same day.
Your certification remains valid for two years. We send renewal reminders so you don’t miss your expiration date, and recertification is equally straightforward. Register today and invest in the confidence that comes from knowing you can respond effectively when someone’s life depends on it.
Register for a class today.
Frequently Asked Questions (FAQ)
What certifications do we offer for healthcare professionals responding to exercise-related emergencies?
We provide BLS, ACLS, and PALS certifications specifically designed for nurses, dentists, EMS personnel, and other healthcare professionals who need current credentials for job compliance and licensure. Our courses combine virtual learning with hands-on skills sessions at over 100 locations across California, and we offer classes daily to fit your schedule.
How quickly can I get certified with your training programs?
We’ve structured our blended learning approach so you can complete coursework on your own timeline and then attend an in-person skills session when it works best for you. Most of our students complete their full certification within days of enrollment, and we maintain a low price guarantee across all our classes.
Do you have training locations near me in California?
We operate over 100 training centers throughout California, including multiple locations in major cities like San Francisco, Los Angeles area, San Diego area, and Sacramento. You can visit our website to find the nearest training location to you and schedule your certification session today.