Table of Contents
- Why Exercise-Related Emergencies Demand Immediate Action
- Recognizing Signs of Sudden Unresponsiveness During Physical Activity
- The Critical First Minutes: Assessing Responsiveness and Airway
- Calling for Help and Positioning the Casualty Safely
- When and How to Perform CPR in Exercise Settings
- Recovery Position and Monitoring Vital Signs
- Preventing Common Mistakes in Fitness Emergency Situations
- How Our Blended CPR Training Prepares You for Real Events
- Workplace and Facility-Specific Emergency Response Plans
- Getting Certified to Respond Confidently to Exercise Emergencies
- Frequently Asked Questions (FAQ)
Why Exercise-Related Emergencies Demand Immediate Action
Exercise-related cardiac emergencies occur without warning. A person can collapse during a fitness class, gym session, or outdoor run and lose consciousness within seconds. When this happens, every moment counts. The first few minutes determine whether someone survives with full brain function or faces permanent disability.
Your immediate response makes the difference. Most exercise-related unresponsiveness stems from sudden cardiac arrest, heat exhaustion, or severe dehydration. These conditions are reversible if treated fast enough. After four to six minutes without adequate oxygen to the brain, permanent damage becomes likely. By ten minutes, survival rates drop dramatically.
We work with healthcare professionals and fitness facility managers across California locations like Sacramento, San Francisco, Oakland, and San Jose who understand this urgency. They know that having trained responders on site transforms outcomes. Your ability to recognize what’s happening and act decisively within the first minutes directly impacts whether someone goes home to their family.
Recognizing Signs of Sudden Unresponsiveness During Physical Activity
Sudden unresponsiveness during or immediately after exercise rarely looks the same twice. However, certain warning signs appear frequently and demand your attention.
Watch for these indicators:
- Loss of consciousness or complete unresponsiveness to voice or physical stimulation
- Gasping or absence of normal breathing
- No pulse or pulse that is difficult to find
- Abnormal skin color (pale, blue, or ashen appearance)
- Unusual body movements or seizure-like activity
- Chest pain or discomfort reported just before collapse
- Excessive sweating followed by sudden collapse
- Confusion or disorientation followed by loss of consciousness
The person may have seemed fine minutes before. Fit, young athletes collapse without warning. Someone recovering from a workout might suddenly lose consciousness. Heat illness can progress rapidly from confusion to complete unresponsiveness.
Your role isn’t to diagnose the specific cause. You don’t need to distinguish between cardiac arrest, heat stroke, or severe dehydration in the moment. What matters is recognizing that unresponsiveness is abnormal and requires immediate emergency action. If someone collapses and doesn’t respond when you call their name or gently tap their shoulder, emergency treatment begins now.
The Critical First Minutes: Assessing Responsiveness and Airway
Your assessment happens in seconds, not minutes. Check responsiveness by calling out to the person and tapping their shoulder firmly. A responsive person will move, speak, or react. An unresponsive person shows no response whatsoever.
Once you confirm unresponsiveness, check the airway immediately. Position the person on their back on a firm surface if they aren’t already. Tilt their head back slightly and lift the chin using one hand while placing your other hand on the forehead. Look inside the mouth for obvious obstructions like food, vomit, or athletic equipment.
If you see a foreign object you can easily remove, do so with your fingers in a sweeping motion. Never probe deeply or perform blind finger sweeps. You could push an obstruction deeper or injure soft tissues.
Check if the person is breathing. Look for chest rise and fall, listen for breath sounds, and feel for air movement. This check takes five to ten seconds. Gasping is not normal breathing. Occasional, irregular gasps during unconsciousness typically indicate cardiac arrest requiring immediate CPR.

If the person is breathing normally and responsive, place them in recovery position and monitor continuously. If they’re unresponsive and not breathing normally, begin CPR immediately. This is your signal that professional help must arrive fast.
Calling for Help and Positioning the Casualty Safely
Activate emergency services immediately when you identify unresponsiveness and abnormal breathing. Call 911 or have someone nearby call while you continue care. Provide the dispatcher with your location, the person’s condition, and whether CPR has begun. If an automated external defibrillator (AED) is available at your facility, mention this to the dispatcher.
While waiting for emergency responders, position the person safely on their back on a hard surface. A gym floor, parking lot, or grass works. Avoid soft surfaces like beds or couches, which make CPR ineffective. Remove tight clothing from the chest area if possible.
If the person is vomiting or has fluid in the mouth, turn their head to the side slightly to prevent aspiration while keeping the airway open. Keep the head tilted and chin elevated. Stay with the person and don’t leave them unattended. Watch for changes in breathing, consciousness, or skin color.
In California facilities across Fresno, Bakersfield, Stockton, and other high-heat regions, exercise-related emergencies often involve heat illness. Even as you call for help, move the person to a shaded area if they’re in direct sunlight. These positioning adjustments support the professional response that’s coming.
When and How to Perform CPR in Exercise Settings
CPR begins when an unresponsive person is not breathing normally. If you feel uncertain about whether breathing is present, err on the side of caution and start CPR. Performing CPR on someone who doesn’t need it causes less harm than withholding it from someone in cardiac arrest.
Hand position matters. Locate the center of the chest, between the nipples. Place the heel of one hand on the sternum, then place your other hand on top, interlacing fingers. Keep your arms straight and shoulders positioned directly above your hands. Push hard and fast at least 2 inches deep at a rate of 100 to 120 compressions per minute. Let the chest recoil completely between compressions.
Compression-only CPR is effective if you’re unable or unwilling to provide rescue breaths. Continue chest compressions until emergency responders arrive, an AED is available, or the person shows signs of life. Don’t stop to check for breathing or pulse frequently. Interruptions reduce effectiveness.
When an AED becomes available, turn it on and follow its prompts. Place pads on the bare chest as directed by the device. Continue CPR while the AED analyzes the heart rhythm. If a shock is needed, ensure no one is touching the person before pressing the shock button. After the shock, resume CPR immediately.
Exercise settings like gyms in Pleasanton, Palo Alto, and throughout the Bay Area increasingly have AEDs on site. Know where your nearest AED is located. Seconds saved in retrieving it improve outcomes significantly.
Recovery Position and Monitoring Vital Signs
If an unresponsive person is breathing normally, place them in the recovery position while waiting for emergency services. This position keeps the airway open and allows fluids to drain from the mouth without obstructing breathing.
Here’s how to position them: Kneel beside the person. Place the arm nearest you at a right angle to their body, palm up. Cross their far leg over the near leg at the knee. Place your hand on their far shoulder and gently roll them toward you onto their side. The upper leg should support the body at the hip and knee. Tilt the head back slightly to maintain airway opening.
Once positioned, monitor breathing and consciousness continuously. Watch their chest rise and fall. Feel for a pulse if trained to do so. Note any changes: Do they regain consciousness? Does breathing become labored? Are there signs of vomiting? Note the time and what you observe.
Keep the person warm if possible by placing a blanket or towel over them. In outdoor or cool environments, this prevents shock. In hot environments like post-exercise settings, avoid overheating. Your priority is maintaining the airway and monitoring their condition until paramedics arrive and take over.
Preventing Common Mistakes in Fitness Emergency Situations

Even well-intentioned responders can make errors that reduce outcome quality. Knowing common mistakes helps you avoid them.
Don’t delay calling 911. Some people hesitate, hoping the person recovers on their own. Every minute without oxygen to the brain matters. Call immediately.
Avoid excessive chest compressions pauses. CPR interrupted for assessment, repositioning, or talking causes survival rates to plummet. Compressions over talking is the approach proven to work.
Don’t give up too early. Paramedics sometimes revive people after extended CPR. Continue compressions until emergency personnel take over or signs of life clearly return.
Never assume someone is “just tired” or “having a panic attack.” Unresponsiveness during or after exercise is an emergency until proven otherwise. Assume cardiac or heat-related causes and act accordingly.
Don’t move the person unnecessarily. Keep them flat on their back unless vomiting or fluid in the airway requires you to turn their head. Unnecessary movement can worsen injuries or disrupt any spontaneous recovery.
Avoid removing athletic equipment hastily. If someone collapses wearing a sports helmet or protective gear, leave it in place. Only remove it if it prevents airway access and you cannot provide care with it on.
How Our Blended CPR Training Prepares You for Real Events
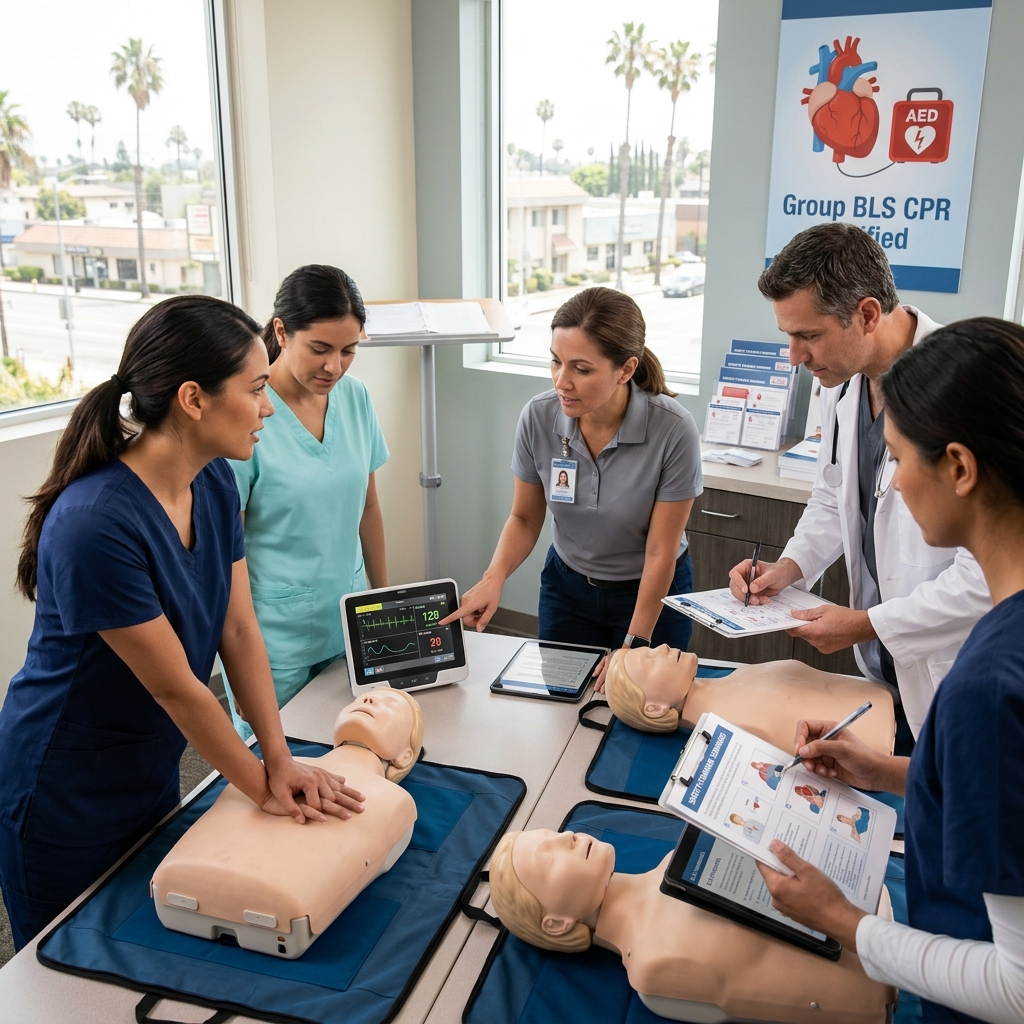
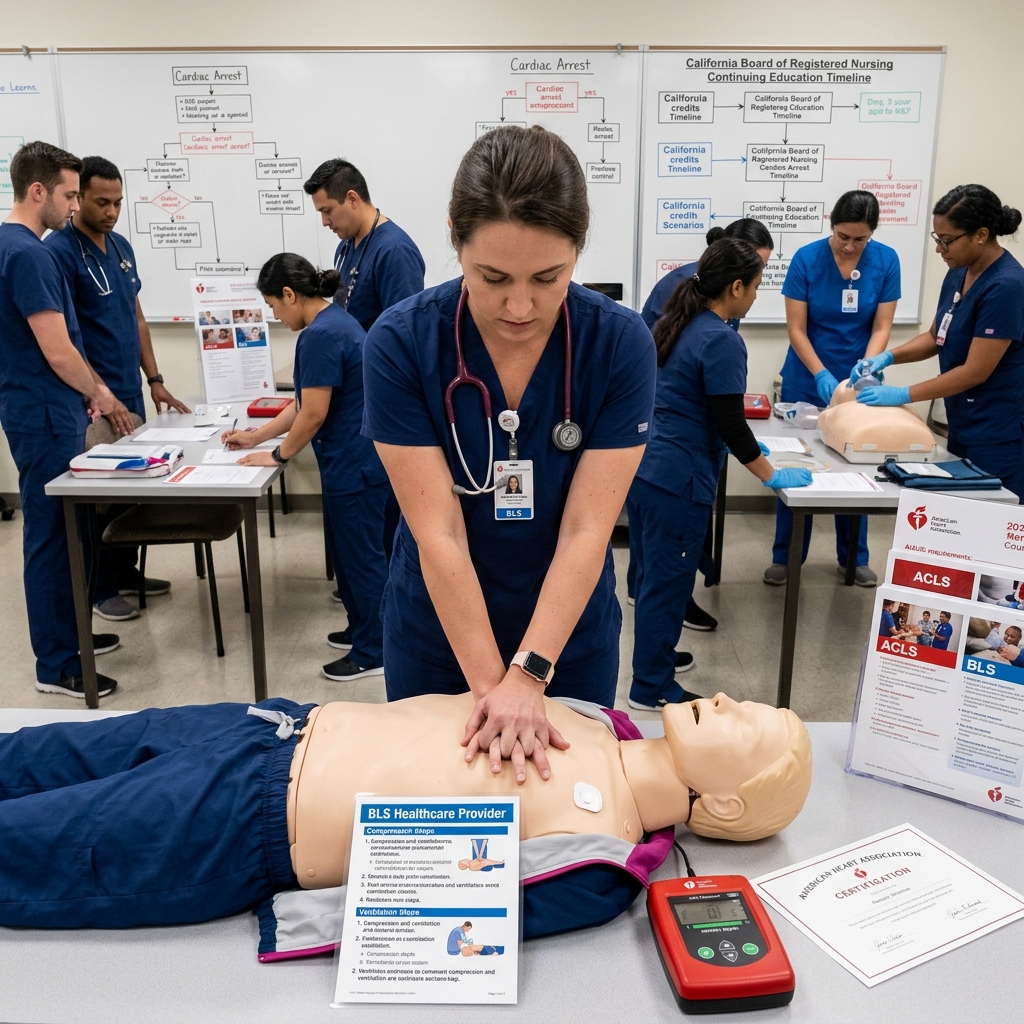
At Safety Training Seminars, we combine virtual learning with hands-on practice specifically designed for real-world fitness emergencies. Our CPR and BLS certification courses include scenario-based training where you practice recognizing unresponsiveness and responding under realistic conditions.
Our instructors emphasize the skills that matter most in exercise settings. You’ll practice chest compressions on manikins that provide feedback so you understand the force and speed required. You’ll work through decision trees: Is the person responsive? Are they breathing? Should CPR start now? By the time you face a real emergency, your muscle memory and decision-making are solid.
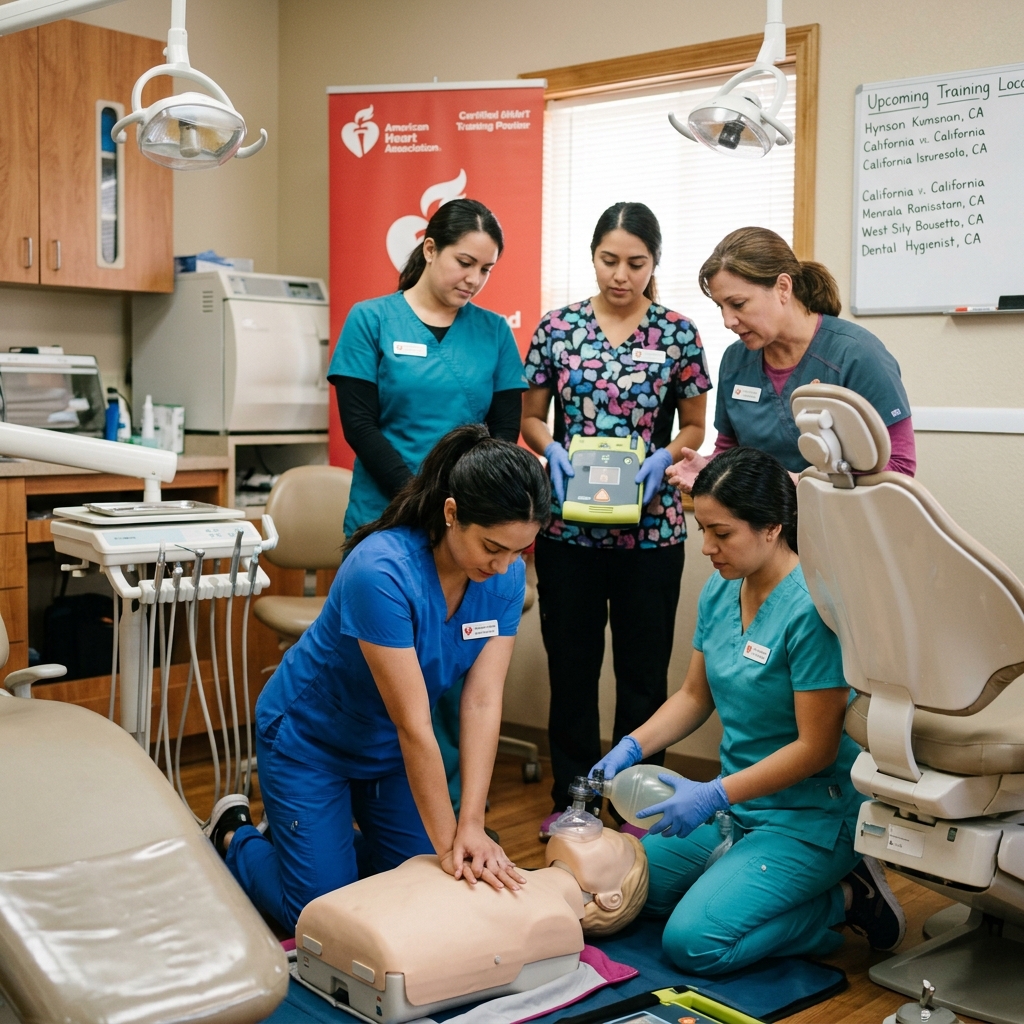
We offer CPR courses at over 100 locations throughout California, including communities like Davis, Modesto, Santa Rosa, and Visalia. Our blended format means you complete online modules on your schedule, then attend a skills session where instructors observe your technique personally. This approach respects your time while ensuring hands-on competency.
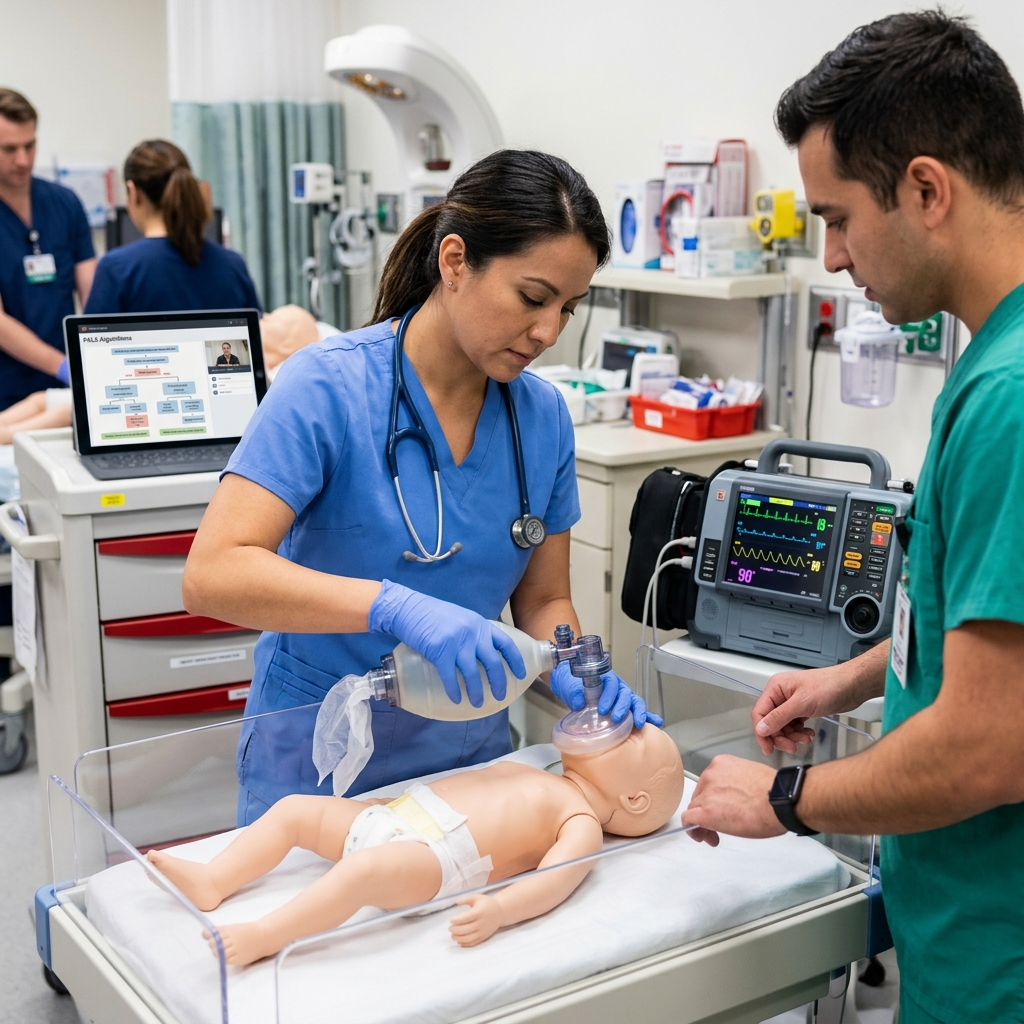
For healthcare professionals like nurses, dentists, and EMS personnel, we offer specialized certifications including Advanced Cardiovascular Life Support (ACLS) and Pediatric Advanced Life Support (PALS). These courses build on CPR fundamentals with advanced rhythm recognition and medication administration relevant to hospital and pre-hospital settings.
Our low price guarantee ensures cost isn’t a barrier to certification. You get instructor experience, real equipment, and verified credentials without paying premium prices. Daily class availability at convenient times means you can schedule training around your shifts and responsibilities.
Workplace and Facility-Specific Emergency Response Plans
Every fitness facility, workplace, and training center should have a documented emergency response plan. As a certified responder, you’re part of this plan.
Review your facility’s plan before an emergency occurs. Where is the AED located? What’s the address dispatchers need? Who is trained in CPR? How do you access the facility’s intercom or alert system to summon help? What’s the quickest route for paramedics to reach your gym or clinic?
Ensure your workplace maintains and regularly tests AEDs. Batteries expire, pads degrade, and devices fail without maintenance. Check your AED monthly and replace batteries and pads according to manufacturer schedules.

Conduct regular drills so your team practices the response sequence. Simulation drills reduce panic and ensure everyone knows their role. During a real emergency, muscle memory and established procedures work faster than figuring things out on the spot.
If your facility operates across multiple locations like our partners in Walnut Creek, San Ramon, or Morgan Hill, ensure each location follows the same basic protocol. Consistency matters. If a staff member works multiple sites, they can apply the same response approach everywhere.
Consider your environment specifically. Outdoor fitness areas need plans for managing heat illness and accessing AEDs quickly. Swimming facilities require water rescue training in addition to CPR. High-altitude training locations face different risks than sea-level gyms. Your plan should address your specific setting.
Getting Certified to Respond Confidently to Exercise Emergencies
Certification provides two critical benefits: legal protection and confidence. In most U.S. states, including California, trained responders who provide CPR in good faith receive legal protection under Good Samaritan laws. Certification documents that you acted within your training.
More importantly, certification builds confidence. You know you can recognize an emergency, you understand the steps, and you’ve practiced the technique. When real pressure arrives, you act decisively instead of freezing.
We recommend CPR and BLS certification for anyone who works in fitness, healthcare, or emergency response. Renewal every two years keeps your skills current and meets professional licensing requirements. Many employers require certification as a job condition. Some positions like nursing and dental hygiene mandate specific certifications like ACLS or PALS.
Starting with our adult and pediatric CPR certification course gives you the foundational skills for most emergency situations. If you work in healthcare, build toward ACLS or PALS based on your specialty. If you work in fitness or coaching, standard CPR plus first aid coverage covers most scenarios.
Our instructors are experienced in real emergency response. They understand the challenges you face in your specific role. Classes in Campbell, Concord, Hayward, and other Northern California locations fill quickly because professionals trust our hands-on approach and flexible scheduling.
Don’t wait until an emergency tests your readiness. Schedule your certification this month. Your next CPR class is available at a location and time that fits your schedule, backed by our low price guarantee and experienced instruction.
Register for a class today.
Frequently Asked Questions (FAQ)
What should I do if someone becomes unresponsive during exercise at our facility?
Our immediate protocol is to ensure your safety first, then assess responsiveness by tapping the person’s shoulders and asking if they’re okay. We recommend calling 911 right away while checking their airway and breathing, then beginning CPR if needed. If you’re trained through our courses, you’ll know exactly how to position them and maintain circulation until emergency responders arrive.
How does our blended training format help me respond effectively to exercise emergencies?
Our combination of virtual instruction and in-person skills sessions means you practice actual CPR techniques on mannequins under our instructors’ guidance, then apply that knowledge in real scenarios. This hands-on approach builds muscle memory and confidence so you can act decisively when an emergency happens, rather than hesitating or second-guessing yourself in a high-stress moment.
Where can I get certified to handle cardiac emergencies in fitness settings?
We offer BLS, ACLS, and specialized certifications at over 100 locations throughout California, with many locations offering daily class options. Our low price guarantee ensures you get certified training without breaking your budget, and we’re available in communities across the state so you can find a convenient location near your workplace or home.