Table of Contents
- Why Proper First Aid Response Matters for Sprains and Fractures
- Understanding the Difference Between Sprains, Fractures, and Severe Falls
- Immediate RICE Protocol: Your First Response to Sprain Injuries
- When to Immobilize and How to Support Fracture Sites
- Recognition and Assessment of Fall-Related Injuries
- Pain Management and Swelling Control in the First Hours
- When to Seek Emergency Medical Care vs Home Treatment
- Recovery Timeline: What to Expect After Sprains and Fractures
- Why Certified First Aid Training Prevents Serious Complications
- Our Blended First Aid Certification Programs Across California
- Getting Certified Today: Flexible Scheduling and Same-Day Credentials
- Frequently Asked Questions (FAQ)
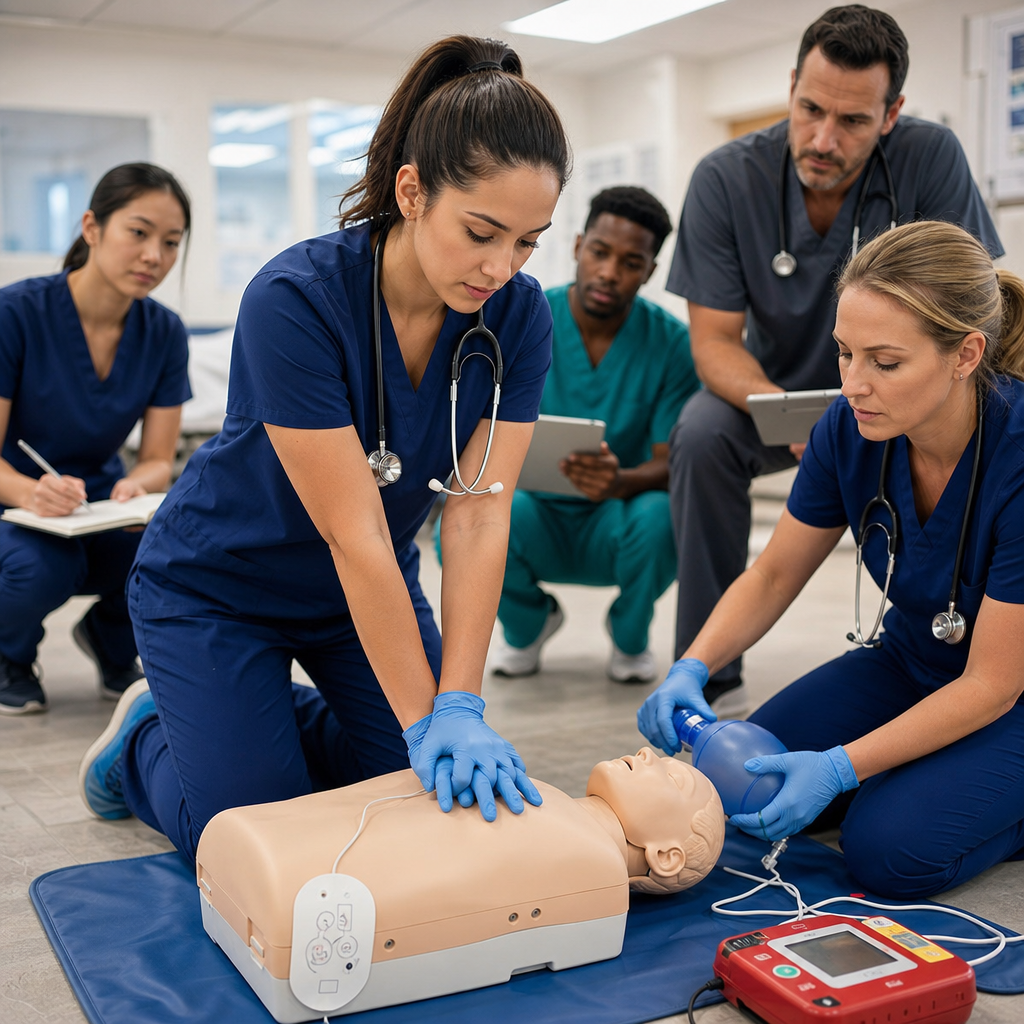
Why Proper First Aid Response Matters for Sprains and Fractures
The first few minutes after a sprain, fracture, or fall determine whether an injury stays manageable or develops into a serious complication. Quick, correct intervention stops bleeding, reduces swelling, and prevents shock. When you respond properly, you preserve function and accelerate healing—sometimes by weeks.
Healthcare professionals like you encounter these injuries regularly. Your patients depend on your knowledge to guide them toward recovery. Workplace injuries affecting nurses, dentists, and EMS personnel demand immediate, confident action. A sprained ankle left untreated can lead to chronic instability. A fractured bone misaligned during transport risks permanent disability. Falls in elderly patients can trigger cascading health crises if initial assessment misses hidden injuries.
The stakes are high because soft tissue damage and bone injuries don’t advertise all their severity upfront. Swelling masks fractures. Pain tolerance varies widely. What looks minor can become major if you delay proper care or apply incorrect technique. Knowing the difference between manageable home care and emergency-level injury is knowledge that saves careers and lives.
Understanding the Difference Between Sprains, Fractures, and Severe Falls
A sprain involves torn or stretched ligaments, the connective tissue linking bones. Sprains range from mild (slight stretch, full function within days) to severe (complete tear, months of rehabilitation). You’ll see swelling, bruising, and limited range of motion. The ankle and knee are most common.
Fractures break bone itself. Signs include severe pain, visible deformity, inability to bear weight, and sometimes a cracking sound at the moment of injury. Fractures demand immobilization to prevent dangerous movement of bone fragments. A person with a fractured wrist won’t be able to rotate their forearm. A broken leg won’t support weight.
Falls create a third category because they often involve multiple injuries simultaneously. An older adult falling from a standing position may fracture a hip, sprain their wrist trying to catch themselves, and hit their head. Falls demand systematic assessment of the entire body, not just the obvious injury. Head injuries, internal bleeding, and spinal trauma are invisible but life-threatening.
The key difference: sprains involve ligaments only, fractures involve bone, and falls require full-body assessment. Your initial observation determines treatment pathway.
Immediate RICE Protocol: Your First Response to Sprain Injuries
RICE stands for Rest, Ice, Compression, and Elevation. This protocol manages pain and swelling in the first 48 to 72 hours after a sprain.
Rest means stopping the activity immediately. Continued movement worsens tissue damage. Encourage your patient to stay off the injured ankle or knee. Rest doesn’t mean complete immobility, but rather avoiding activities that cause pain.
Ice reduces blood flow to the injury, slowing swelling and numbing pain. Apply ice for 15 to 20 minutes every 2 to 3 hours during the first day. Use a bag of frozen peas or ice wrapped in a thin cloth. Never apply ice directly to skin, as this risks cold burns. Ice loses effectiveness after the first 72 hours because swelling has already peaked.
Compression uses an elastic bandage or wrap to limit swelling. Wrap snugly but not so tight that you cut off circulation. Your patient should feel gentle pressure, not numbness or tingling. Compression stabilizes the joint and reduces fluid accumulation in surrounding tissues.
Elevation combats gravity. Have your patient raise the injured limb above heart level using pillows or cushions. Gravity naturally draws fluid away from the injury site, reducing swelling faster. Even 30 minutes of elevation every few hours makes measurable difference.
Start RICE immediately. The sooner you apply this protocol, the better the outcome. Most mild sprains respond well within two weeks.
When to Immobilize and How to Support Fracture Sites
Fractures require immobilization to prevent bone fragments from moving. Movement causes additional soft tissue damage, increases pain, and delays healing. Immobilization protects the injury during transport and initial treatment.
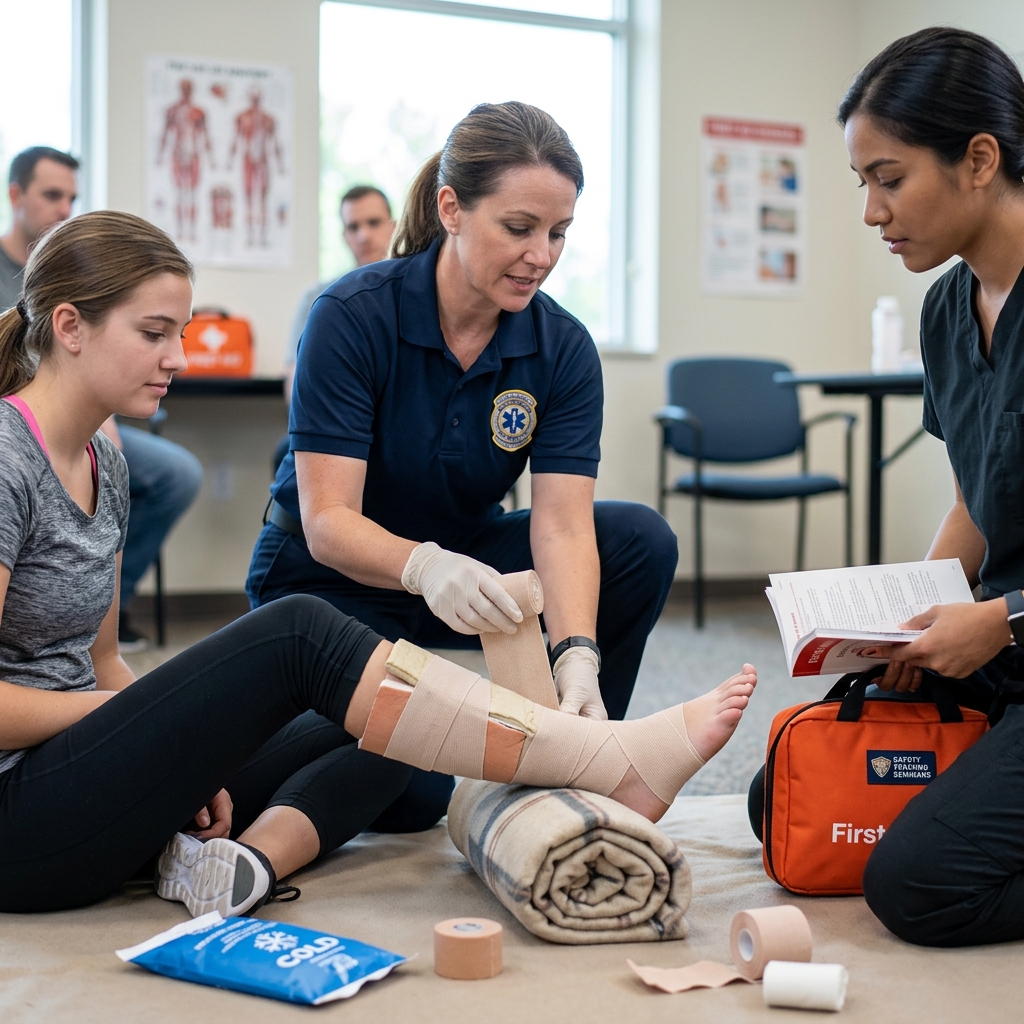
Use a sling for upper arm or shoulder fractures. Support the injured arm across the body, holding it steady against the torso. This prevents any independent movement. For wrist or hand fractures, a padded splint supporting the wrist in neutral position works well. Avoid extreme bending.
Lower leg fractures need rigid support. Padding is essential to prevent skin damage. Wrap the leg with blankets or towels, then secure gently with cloth strips. Don’t apply a tourniquet-like compression. The goal is stability without cutting off blood supply.
Spinal fractures demand extra caution. If you suspect spinal injury from a fall, keep the person lying flat and still. Do not move them unless absolutely necessary to escape immediate danger. Movement risks paralysis. Movement risks catastrophic damage.
For all fractures, the golden rule is immobilization before transport. A person with a fractured ankle who walks on it will cause severe additional injury. Even gentle movement can worsen outcomes. Immobilize first, then arrange transport to medical evaluation.
Check circulation after immobilization. Fingers or toes should remain warm and maintain normal color. If they turn pale or purple, loosen the immobilization slightly.
Recognition and Assessment of Fall-Related Injuries
Falls require systematic head-to-toe assessment because injuries cluster and overlap. Start by checking responsiveness. Can they talk clearly? Do they understand your questions? Confusion or difficulty speaking signals possible head injury.
Inspect the head and neck. Look for cuts, bumps, or blood. Ask about pain in the neck or upper back. If they hit their head or have any neck pain, assume spinal injury until proven otherwise. Keep the spine still.
Check both arms and legs for deformity, swelling, or inability to move. Ask your patient to gently wiggle fingers and toes. Can they feel sensation? Loss of sensation means nerve involvement.
Palpate the ribs, abdomen, and pelvis gently. Pain here might indicate internal injury not visible on the surface. Severe abdominal pain after a fall warrants immediate emergency evaluation even if the person is conscious and alert.
Ask about the fall itself. How far did they fall? Did they lose consciousness? Do they remember hitting their head? These details help you gauge severity. A 75-year-old who fell from standing and can’t get up has very different risk profile than a 30-year-old who tripped stepping off a curb.
Falls in elderly patients are particularly dangerous. Bones are more fragile. Falls that seem minor can fracture a hip or pelvis. Anticoagulant medications common in older adults increase bleeding risk. What looks like a simple fall deserves careful evaluation.
Pain Management and Swelling Control in the First Hours
Pain and swelling go hand-in-hand in soft tissue injuries. Swelling causes pain, and pain triggers more swelling. Breaking this cycle early prevents complications.
Ice remains the gold standard for the first 72 hours. Temperature reduces metabolic activity in injured tissues, limiting inflammation. Most facilities across California, from Folsom to Petaluma, recommend ice as first-line management.
Over-the-counter non-steroidal anti-inflammatory drugs (NSAIDs) like ibuprofen reduce both pain and inflammation. Dosing according to package directions helps. NSAIDs work best when started early, within the first few hours of injury.
Compression and elevation work together to control swelling. Gravity and gentle pressure both prevent fluid accumulation. Your patient should notice reduced swelling within hours when these methods are applied consistently.
Position matters. Lying flat with the injured limb elevated beats sitting upright. The higher above heart level, the more effective the elevation. Pillows supporting an injured ankle or knee are simple but effective tools.
Avoid heat in the first 72 hours. Heat increases blood flow to the injury, worsening swelling. Heat feels soothing psychologically, but it delays healing. After 72 hours, when acute swelling has peaked, gentle heat can help muscle relaxation.
When to Seek Emergency Medical Care vs Home Treatment
Minor sprains, where the person can bear some weight and has normal sensation, typically respond to home care. Pain should improve daily. Swelling should decrease over the first week.

Fractures always require professional evaluation. X-rays confirm the type and severity of break. Even suspected fractures warrant medical assessment. Never assume a fracture won’t be serious.
Seek emergency care if your patient has any of these warning signs after a fall:
- Loss of consciousness, even briefly
- Severe headache that worsens
- Confusion, slurred speech, or difficulty understanding
- Severe abdominal pain
- Inability to move a limb despite trying
- Numbness or tingling below the injury
- Pale, cold, or blue-colored fingers or toes
- Severe, uncontrolled bleeding
- Visible deformity suggesting fracture
Falls in elderly patients warrant careful evaluation even when symptoms seem mild. Hip fractures often aren’t obvious immediately. An older person who fell and now walks differently or can’t bear weight needs imaging.
A sprain that doesn’t improve within a week despite RICE protocol suggests a more severe injury. Persistent swelling or inability to bear weight after 48 hours indicates professional assessment is needed.
Recovery Timeline: What to Expect After Sprains and Fractures
Mild ankle sprains typically heal within 2 to 3 weeks with consistent RICE protocol. Moderate sprains need 4 to 6 weeks. Severe sprains, involving complete ligament tears, may require physical therapy lasting months.
Fractures heal on a bone-specific timeline. Hand and wrist fractures typically immobilize for 3 to 6 weeks, then graduated strengthening. Ankle fractures need 6 to 8 weeks of immobilization. Hip fractures in older adults require months of recovery and intensive rehabilitation.
Early mobilization within pain limits speeds recovery. After initial acute swelling peaks, gentle movement prevents stiffness and maintains circulation. A sprained ankle might progress from complete rest to gentle ankle circles by day 3 or 4.
Physical therapy accelerates healing. Licensed therapists guide progressive strengthening that rebuilds stability and function. Someone who skips therapy after a severe ankle sprain faces higher risk of re-injury.
Swelling can persist for weeks or months, especially with fractures. Don’t interpret lingering swelling as a sign of poor healing. Bone remodeling takes time. Soft tissue remodeling takes time.
Return to full function happens gradually. An athlete who injured an ankle shouldn’t resume sport immediately after the immobilization period ends. Gradual progression from walking to jogging to sport-specific movements prevents re-injury.
Why Certified First Aid Training Prevents Serious Complications
Certification teaches you decision-making frameworks that prevent mistakes. You learn the difference between injuries you can safely manage and those requiring emergency transport. You learn immobilization techniques that actually work. You learn assessment patterns that catch hidden injuries.
Training also builds confidence. In high-stress moments after an injury, knowing your skills are validated by certification lets you act decisively rather than freezing. Your patients recognize your authority and follow your guidance.
Certified responders know local protocols. Training includes updates on equipment available in your setting. You’ll know exactly what’s in your first aid kit and how to use it effectively.
Perhaps most importantly, certification teaches the legal and ethical frameworks governing first aid response. You’ll understand scope of practice, liability protection, and documentation. You’ll know when you must act and when you must refer.
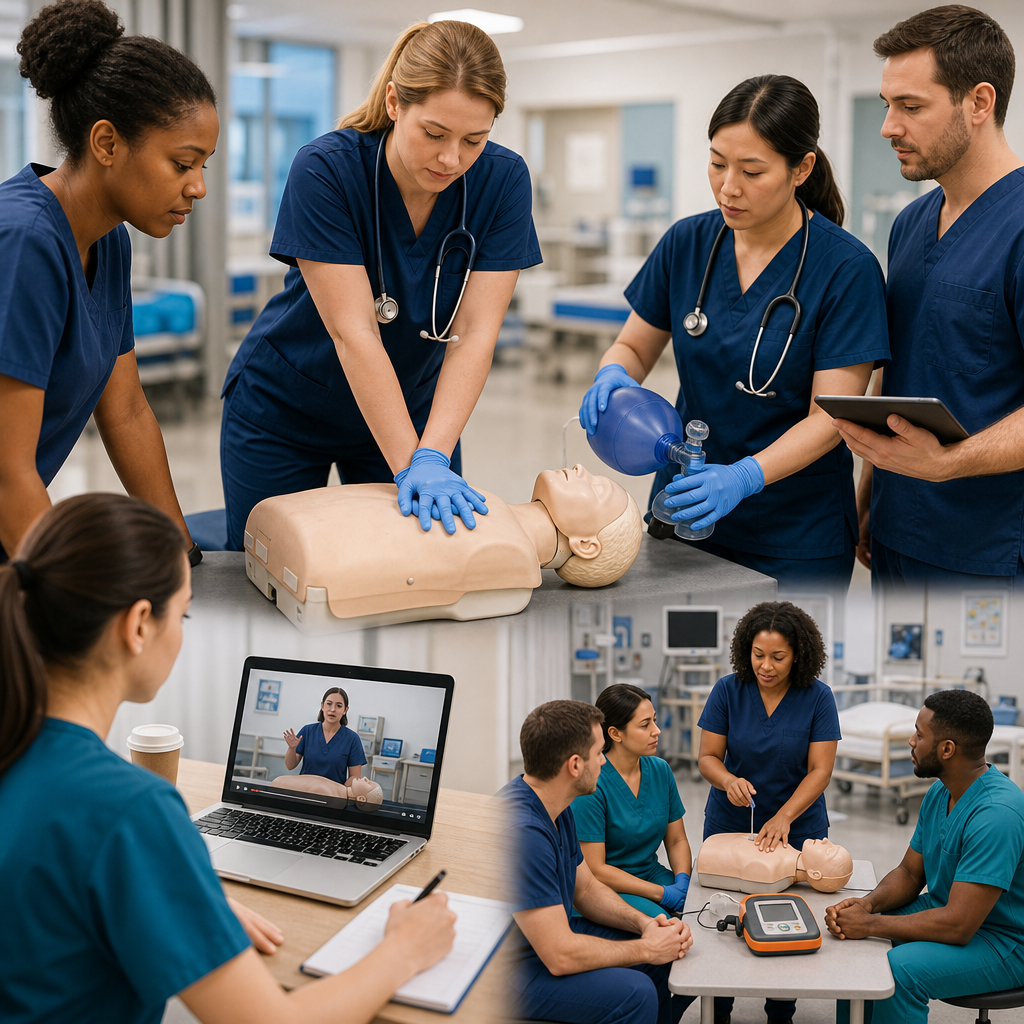
Our first aid certification programs teach hands-on skills with classroom knowledge. You’ll practice immobilizing fractures on training mannequins. You’ll simulate fall assessment on actors. You’ll learn current guidelines and best practices.
Healthcare professionals working in California, whether in Sacramento, San Jose, Oakland, or San Francisco, benefit from certification tailored to your workplace environment. Your patients receive better care when you’re trained and confident.
Our Blended First Aid Certification Programs Across California
We combine in-person skills practice with flexible online learning. You attend one focused session where you’ll practice immobilization, RICE protocol, fall assessment, and other hands-on techniques. Our instructors correct your technique in real-time. You’ll work with realistic scenarios and equipment.

Online modules cover theory, anatomy, and decision-making frameworks. You can complete these on your schedule, from Bakersfield to Redding, from Visalia to Vallejo. No rushing. No one-size-fits-all pacing.
Over 100 training locations throughout California means you’ll find a class near you. Whether you work in Concord, Pleasanton, Davis, or Sunnyvale, we have accessible scheduling. Many locations offer daily sessions, including evenings and weekends.
We offer specialized certifications for healthcare providers. Our ACLS and PALS programs go deeper into cardiac emergencies. Our neonatal resuscitation program covers NRP skills. These advanced certifications meet licensing requirements for nurses, dentists, EMS personnel, and other healthcare professionals.
Corporate group training is available with discount pricing. If your workplace needs multiple staff certified, we arrange on-site or nearby group sessions. Your entire team gets same-day credentials.
Our low price guarantee ensures you’re not overpaying. We’re transparent about costs. No hidden fees. No surprise charges.
Getting Certified Today: Flexible Scheduling and Same-Day Credentials
Scheduling is straightforward. Visit our website to browse available classes in your location. Most areas offer multiple sessions weekly. Pick the time that fits your calendar. Online portions can start immediately after you register.
In-person skills sessions typically last 2 to 4 hours depending on the certification level. You’ll receive your credential same-day upon successful completion. No waiting for credentials to arrive by mail.
Same-day credentials mean you can start using your certification immediately. If your employer requires current certification, you’re covered the moment you finish the course. No gap between training and credentials.
We accept all payment methods. Flexible payment plans are available for group trainings. Our transparent pricing and low price guarantee mean no surprises.
Your next step: identify which certification you need. Healthcare professionals in California typically need standard first aid certification at minimum. Many need BLS or ACLS as well. Check your employer’s requirements.
Browse our available classes in your area. Locations like San Francisco, Berkeley, Fremont, San Jose, Sacramento, and dozens of other California cities have ongoing sessions. Register for the class that fits your schedule. Complete your online portion at your own pace.
We’re here to support your professional development and your patients’ safety.
Register for a class today.
Frequently Asked Questions (FAQ)
What’s the difference between how we treat a sprain versus a fracture in the first aid response?
We treat sprains and fractures differently because sprains involve stretched or torn ligaments while fractures involve broken bones. For sprains, we apply our RICE protocol (Rest, Ice, Compression, Elevation) to reduce swelling and pain. For fractures, we prioritize immobilization first to prevent further bone displacement, then apply ice and elevation while keeping the area completely still until medical professionals can assess the injury.
Why does our certified first aid training emphasize recognizing when to seek emergency care for falls?
We emphasize emergency recognition because falls can cause hidden injuries that worsen without proper medical evaluation. Our training teaches you to identify red flags like severe pain, inability to move a limb, visible deformity, loss of consciousness, or head and neck involvement. We show you exactly when home treatment is sufficient and when immediate emergency care becomes critical to prevent complications like internal bleeding or spinal damage.
How can we help you maintain your required certifications while managing your busy healthcare schedule?
We offer blended learning programs that combine virtual instruction with in-person skills sessions at over 100 California locations, so you can study flexibly and practice hands-on techniques when it works for you. Our daily BLS certification courses and multiple training sites mean we can fit your renewal schedule around your work demands without compromising the quality of your preparation.