Table of Contents
- Why Exercise-Related Collapses Happen More Often Than You Think
- The Critical First Moments: What You Need to Do Immediately
- Assessing Responsiveness and Checking for Breathing
- The Role of CPR in Exercise Emergency Response
- When to Call Emergency Services and What Information to Provide
- Recovery Position and Monitoring Vital Signs
- Common Mistakes People Make During Exercise Emergencies
- Our Comprehensive Emergency Response Training for Active Individuals
- How Our Blended Learning Approach Prepares You for Real Situations
- Getting Your Certification Today at One of Our California Locations
- Frequently Asked Questions (FAQ)
Why Exercise-Related Collapses Happen More Often Than You Think
When someone collapses during or immediately after a workout, the minutes that follow determine outcomes. Whether you’re a nurse managing a patient, an EMS professional responding to calls, or a gym-goer who happens to be nearby, knowing how to help an unresponsive person after exercise is a life-saving skill. We’ve trained thousands of healthcare professionals and active individuals across California to recognize and respond to exercise-related emergencies with confidence and precision.
Exercise stress can trigger sudden medical events that seem to come without warning. The combination of elevated heart rate, exertion, and existing cardiovascular conditions creates a perfect storm for collapse. Common causes include arrhythmias (irregular heartbeats), heat exhaustion, dehydration, undiagnosed heart conditions, and sudden cardiac arrest.
What surprises many people is that exercise-related emergencies don’t exclusively affect those with known risk factors. Young, seemingly healthy athletes collapse every year from undetected heart defects or electrolyte imbalances. Older adults pushing harder than usual, weekend warriors returning to activity after months off, and individuals taking certain medications all face elevated risk.
The American Heart Association emphasizes that fitness enthusiasts, athletes, and healthcare workers must understand these risks. Recognizing that collapse can happen to anyone motivates us to stay prepared rather than assume it won’t occur in our communities.
The Critical First Moments: What You Need to Do Immediately
The first 30 to 60 seconds after someone collapses are absolutely critical. Your immediate actions directly influence survival rates.
Start by ensuring the scene is safe for you and the collapsed person. Move them away from equipment, traffic, or other hazards if it’s safe to do so. Then follow these essential steps:
- Check for responsiveness by tapping their shoulders and shouting “Are you okay?”
- Call for help immediately and request an automated external defibrillator (AED)
- Position the person on their back on a firm, flat surface
- Begin assessing their breathing while preparing to act
If you’re at a facility like a gym or community center, a colleague should locate the AED while you remain with the person. Time is not your friend in these situations, and every second of delay reduces the chance of successful resuscitation. In outdoor settings, call 911 first and describe your location clearly so responders can find you.
Assessing Responsiveness and Checking for Breathing
Responsiveness assessment takes only seconds but gives you critical information. Gently tap the person’s shoulders and speak loudly: “Can you hear me? Are you okay?” Watch for any reaction, eye movement, or response to your voice.

Once you’ve confirmed unresponsiveness, check for normal breathing. Look at their chest, listen for breath sounds, and feel for air movement for no more than 10 seconds. Many untrained responders waste precious time here, unsure what “normal breathing” sounds like. Gasping, gurgling, or irregular breathing patterns should be treated as absence of normal breathing.
If the person is unresponsive and not breathing normally, they require immediate CPR (cardiopulmonary resuscitation). Don’t second-guess yourself or wait for signs of life. The sooner you begin chest compressions, the better their chance of survival. Hesitation in these moments can be fatal.
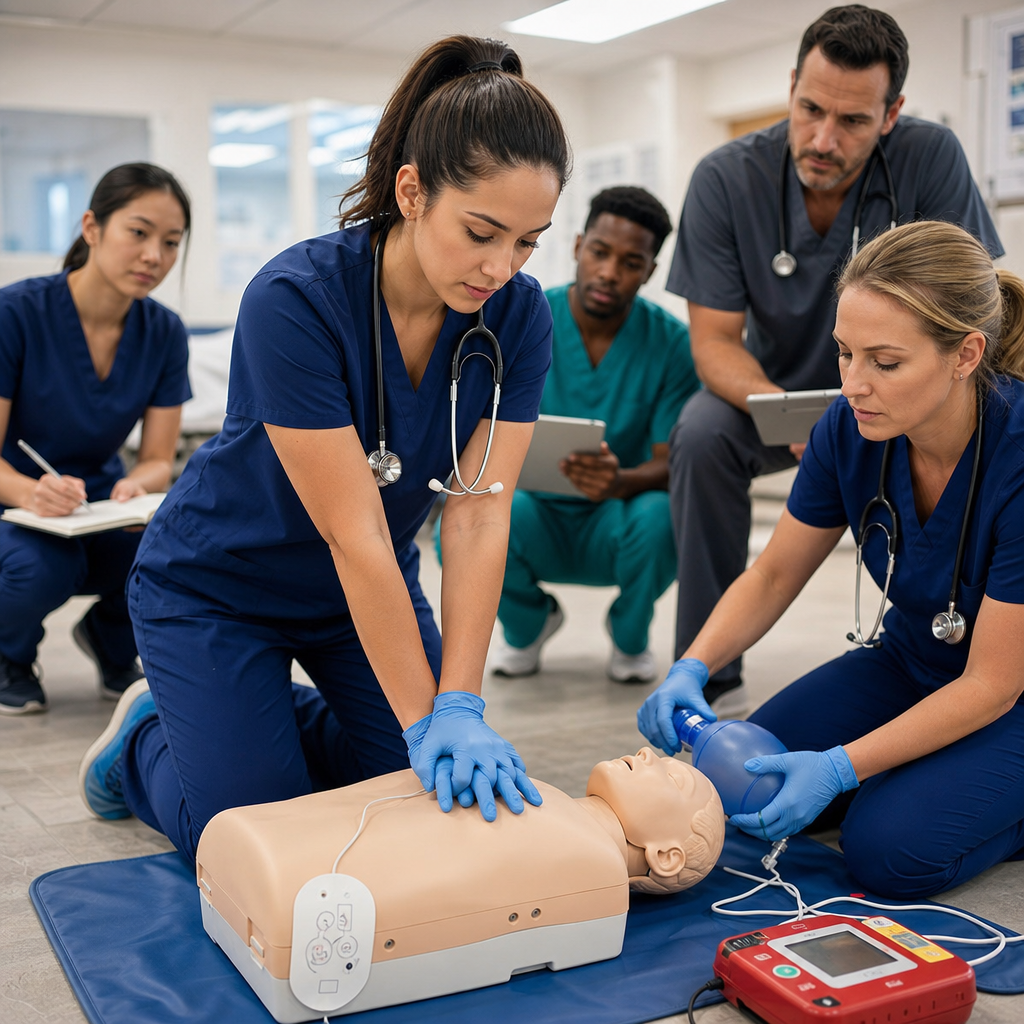
The Role of CPR in Exercise Emergency Response
CPR serves a single, vital purpose: maintaining blood flow to the brain and heart until defibrillation or advanced medical care arrives. When someone collapses from sudden cardiac arrest, their heart has stopped pumping effectively. CPR buys time.
For an unresponsive person after exercise who isn’t breathing normally, begin chest compressions immediately at a rate of 100 to 120 compressions per minute. Place the heel of one hand on the center of the chest, place your other hand on top, and push hard and fast. Compress at least 2 inches deep for adults. If you’re trained and comfortable providing rescue breaths, continue the standard 30:2 ratio (30 compressions to 2 breaths). If rescue breaths aren’t your comfort level, hands-only CPR with continuous chest compressions is equally effective.
Continue CPR until an AED arrives, emergency responders take over, or the person starts breathing and becomes responsive. Fatigue is real, so if multiple people are present, switch compressors every 2 minutes. CPR is physically demanding, and quality matters more than endurance from a single person.
When to Call Emergency Services and What Information to Provide
Call 911 (or have someone call immediately) the moment you determine the person is unresponsive and not breathing normally. Don’t wait for the AED. Don’t wait for additional help. Call now.
When you reach the dispatcher, provide this information clearly:
- Your exact location and facility name (gym, park, outdoor trail)
- That an unresponsive person is not breathing normally
- That CPR is in progress or an AED is being retrieved
- Any known medical history or medications the person is taking
- The person’s approximate age and gender
- Clear landmarks or entrance directions for responders
Dispatchers can guide you through CPR if you haven’t received training, though professional certification is far more effective. Stay on the line and follow their instructions. They’ll coordinate with paramedics and provide real-time guidance based on what you observe.
Recovery Position and Monitoring Vital Signs
If the person regains consciousness and begins breathing normally before emergency responders arrive, place them in the recovery position. Turn them onto their side with their head tilted back slightly to keep the airway open. Bend one leg for stability, and position their arm so their head rests comfortably.
Monitor their breathing, consciousness level, and responsiveness continuously. Watch for changes in skin color, temperature, or responsiveness. If they vomit, tilt their head to the side so they don’t aspirate. Keep them calm and reassure them that help is on the way.

Even if the person seems fine and regains full consciousness, they must still receive medical evaluation. What triggered the collapse might not be immediately apparent. Healthcare professionals, nurses, and dentists understand that post-event assessment by emergency medicine specialists is non-negotiable for liability and patient safety.
Common Mistakes People Make During Exercise Emergencies
Delay in calling 911 tops the list. People hesitate, assume the person will recover on their own, or think they should wait to see if consciousness returns. Call immediately. There’s no downside to summoning help early and every downside to calling late.
Incorrect CPR technique wastes critical minutes. Compressions that are too shallow, too slow, or insufficiently forceful don’t maintain adequate circulation. This is why professional training through certified instructors matters. You need hands-on practice with feedback to build muscle memory.
Failing to use an AED is another critical error. Some people don’t know where the nearest AED is located or hesitate to use one. AEDs are designed for lay responders; they provide clear voice prompts and won’t shock someone who doesn’t need it. Using an AED alongside CPR dramatically improves survival outcomes.
Misinterpreting agonal gasping as normal breathing causes responders to delay CPR. Gasping isn’t breathing. If you’re uncertain, begin CPR. The harm from unnecessary compressions is far less than the harm from delayed CPR.
Finally, moving an unresponsive person unnecessarily or failing to protect their cervical spine during transport puts them at additional risk. Keep them still until trained paramedics arrive, especially if you suspect a head or spinal injury from the collapse itself.
Our Comprehensive Emergency Response Training for Active Individuals
We offer BLS (Basic Life Support) and CPR certification courses specifically designed for healthcare professionals and active individuals who want genuine competency, not just a card. Our instructors bring real emergency response experience from nursing, EMS, and critical care backgrounds. They teach what actually works in the field, not just theory.
Our courses include extensive hands-on practice with manikins, real-world scenarios based on actual emergencies, and immediate feedback on your technique. You’ll practice compressions, airway management, rescue breathing, and AED operation until you’re confident and competent. We offer daily BLS Certification courses at over 100 training locations throughout California, including Sacramento, San Jose, San Francisco, and many communities in between.
For nurses and dentists who need ACLS (Advanced Cardiovascular Life Support) or other specialized certifications, we provide those as well. Our healthcare-specific training acknowledges your professional requirements and builds on the foundation you already have.
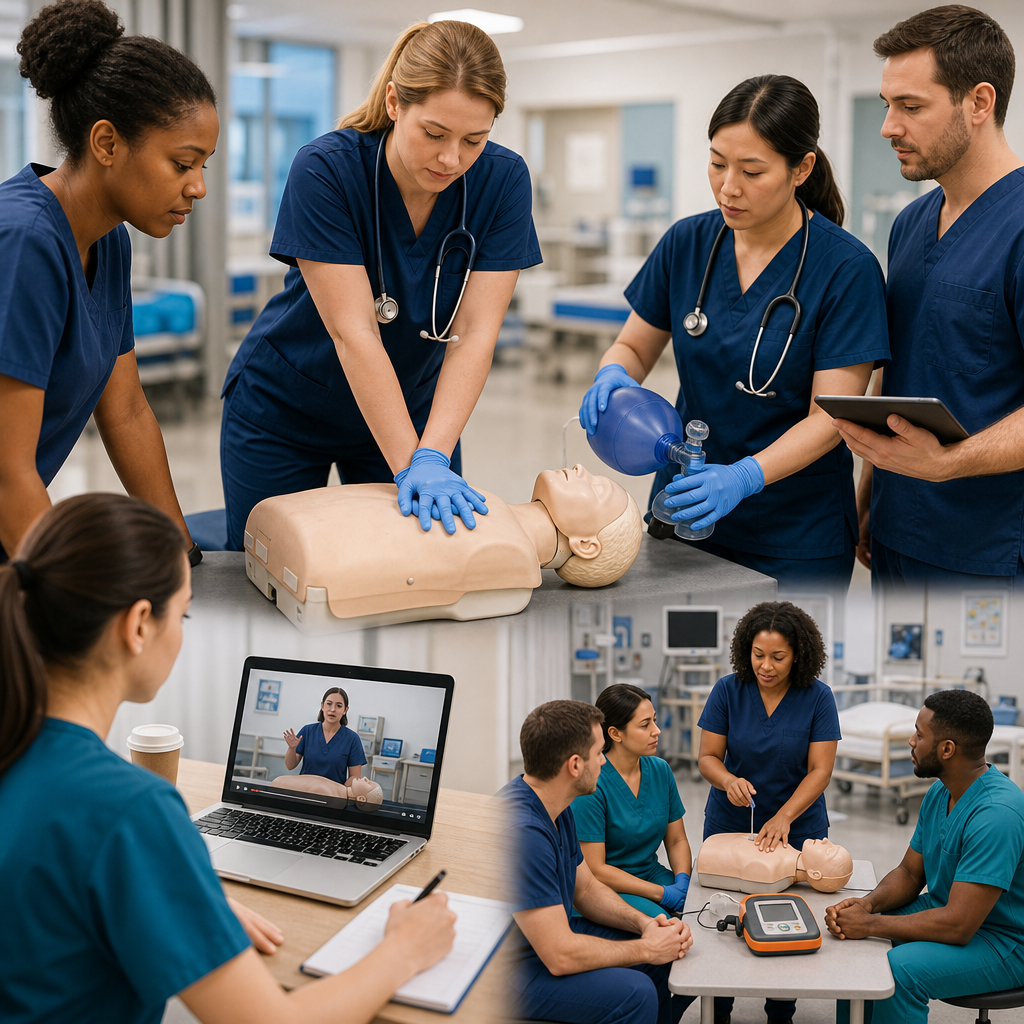
How Our Blended Learning Approach Prepares You for Real Situations
We combine online learning modules with in-person skills sessions to maximize your understanding and retention. You’ll complete the knowledge components at your own pace, then attend a hands-on session where our certified instructors watch you perform CPR, use an AED, and respond to realistic scenarios. This blended approach respects your schedule while ensuring genuine competency.
The in-person skills portion is where real learning happens. You can’t practice CPR on a manikin online, and you can’t build the muscle memory and confidence you need through a video alone. Our instructors provide corrective feedback, adjust your hand placement, and watch your technique improve during the session. When you finish, you’re not just certified; you’re genuinely prepared.

We also offer corporate group training and discounted pricing for healthcare organizations, fitness facilities, and worksites. If you work in a facility where multiple staff members need certification, we can bring training to your location or provide significant discounts for group enrollment.
Getting Your Certification Today at One of Our California Locations
You can enroll in CPR and BLS courses right now through our website. We have classes available daily across California, with convenient locations in Alameda, Bakersfield, Berkeley, Campbell, Davis, Fairfield, Folsom, Fresno, Hayward, Livermore, Los Gatos, Modesto, Morgan Hill, Napa, Oakland, Palo Alto, Petaluma, Pleasanton, Redwood City, Rocklin, Roseville, and many more communities.
If you’re in the Santa Rosa area, CPR and BLS in Santa Rosa courses are available with flexible scheduling. We also maintain California locations throughout the state, so you can find a training center near your home or workplace.
Our low price guarantee means you won’t find more affordable certification elsewhere without compromising quality or instructor experience. Choose your location, select your course date, and complete your online component whenever it fits your schedule. Then attend your in-person skills session and leave as a certified responder ready to help.
The knowledge you gain in this training could save someone’s life at the gym, on a running trail, or in your workplace. When you witness an unresponsive person after exercise, you’ll know exactly what to do, and that confidence matters. Register today and join thousands of healthcare professionals across California who trust us for their life-saving certifications.
Register for a class today.
Frequently Asked Questions (FAQ)
What should I do in the first moments when someone collapses during exercise?
Your immediate priority is to check responsiveness by tapping their shoulders and shouting to see if they react. If unresponsive, call 911 right away and locate the nearest AED while beginning CPR if you’re trained. We emphasize that those critical first 30 seconds can mean the difference between survival and permanent damage, which is why we drill these steps repeatedly in our courses.
How do I know if an exercise-related collapse requires CPR?
After calling 911, check if the person is breathing normally by tilting their head back and observing their chest for 10 seconds. If they’re not breathing or only gasping, start chest compressions immediately at a rate of 100-120 compressions per minute until emergency responders arrive or an AED is available. We teach you how to recognize these life-threatening situations so you can act with confidence rather than hesitation.
Why should healthcare professionals get specialized training beyond basic CPR?
Our ACLS and PALS certifications equip you with advanced protocols for recognizing underlying cardiac or respiratory causes specific to exercise emergencies that basic CPR doesn’t cover. Since you encounter these situations professionally, we provide the deeper knowledge your license requires and your patients deserve, with courses available daily across our 100+ California locations.